Comprehensive Strategies for Effective Management of Type 2 Diabetes
This comprehensive article explores the latest strategies in managing type 2 diabetes, including diet, physical activity, blood sugar monitoring, and medical treatments. It emphasizes the importance of personalized care, practical lifestyle tips, and advanced medical interventions like insulin therapy and bariatric surgery, helping patients achieve better glycemic control and reduce complications. This guide provides actionable insights for anyone seeking effective diabetes management solutions.
Effective Approaches to Controlling Type 2 Diabetes
Managing type 2 diabetes requires a multifaceted approach that includes lifestyle modifications, dietary strategies, medication management, and consistent blood sugar monitoring. With proper care, individuals with this condition can achieve better glycemic control, reduce complications, and improve their quality of life. This article delves into the latest techniques, dietary recommendations, physical activity tips, and medical interventions that are transforming diabetes management today.
While there is no definitive diet that guarantees a cure for type 2 diabetes, certain eating habits can significantly support disease management and overall health. Emphasizing foods that are low in fats, rich in fiber, and have a low glycemic index can help regulate blood sugar levels effectively. Incorporating whole grains, fresh fruits, and vegetables into daily meals is highly recommended. Conversely, reducing consumption of red meats, refined sugars, and processed foods helps prevent blood sugar spikes and contributes to better health outcomes.
Foods with a low glycemic index (GI) are especially beneficial because they release glucose slowly into the bloodstream, preventing rapid increases in blood sugar. Choosing low-GI foods such as legumes, oats, and certain fruits assists in maintaining stable blood glucose levels over time. Understanding and utilizing the glycemic index is an essential part of an effective diabetes management plan.
Glycemic index measures how quickly carbohydrate-containing foods raise blood sugar after eating. High-GI foods like white bread and sugary snacks lead to rapid spikes, whereas low-GI options such as oats, beans, and most vegetables promote gradual sugar absorption. Opting for high-fiber, low-GI foods is a key strategy in controlling blood glucose levels.
Physical activity
Engaging in regular exercise plays a crucial role in managing type 2 diabetes. Consistent physical activity helps improve insulin sensitivity, promote weight loss, and stabilize blood sugar levels. Before starting any exercise routine, consulting your healthcare provider is essential to ensure safety and personalize the plan. Activities like brisk walking, cycling, dancing, swimming, or even resistance training can be both enjoyable and effective. Aiming for at least 150 minutes of moderate exercise each week—such as five 30-minute sessions—is recommended. Incorporating strength training and flexibility exercises like yoga can further enhance results. It’s important to monitor blood sugar levels before and after physical activity, especially for those on insulin or other medications to prevent hypoglycemia. Snacking appropriately before exercise can also help maintain stable blood sugar levels.
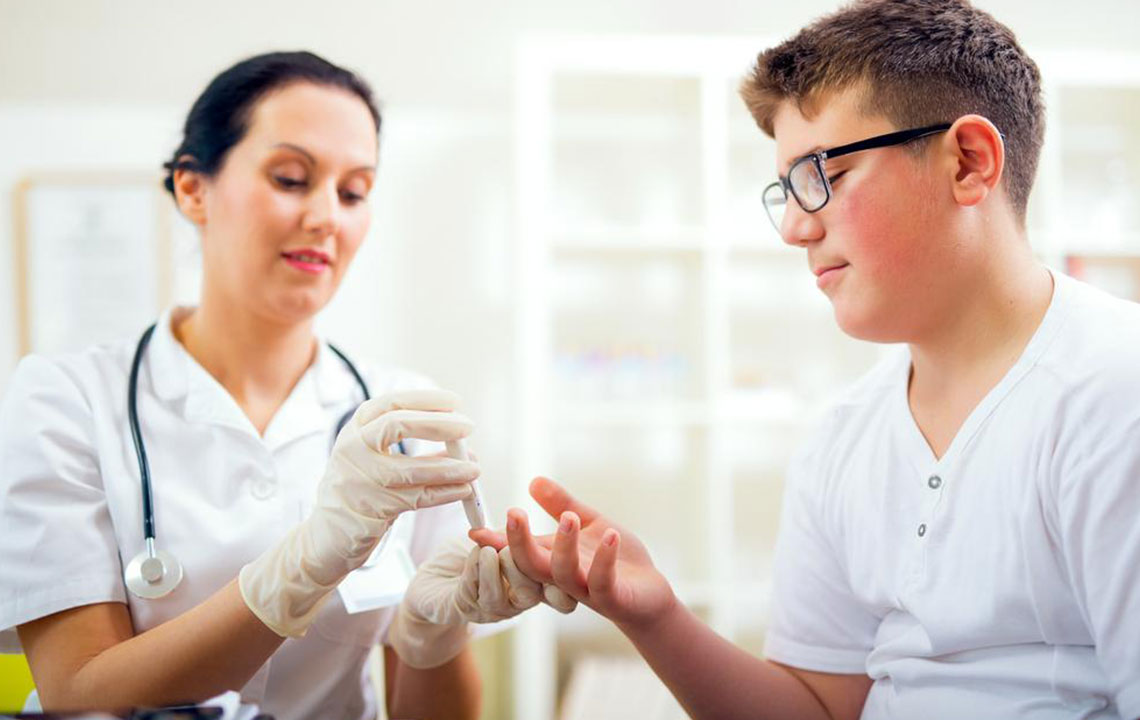
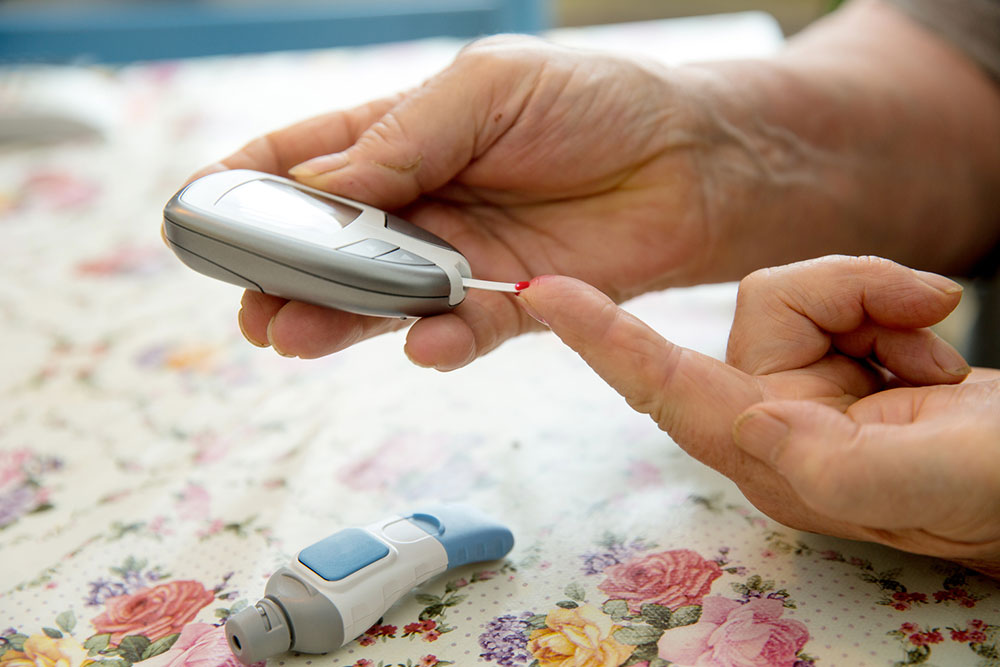
Monitoring blood sugar levels precisely is vital for effective diabetes management. Regular testing allows individuals to understand how their lifestyle, diet, medication, and activity impact their blood glucose. For those on insulin therapy, frequent measurements—such as before and after meals, or before physical activity—are necessary to prevent dangerous fluctuations and hypoglycemia. Keeping a detailed log helps healthcare providers tailor treatment plans more effectively, ensuring optimal control of the disease.
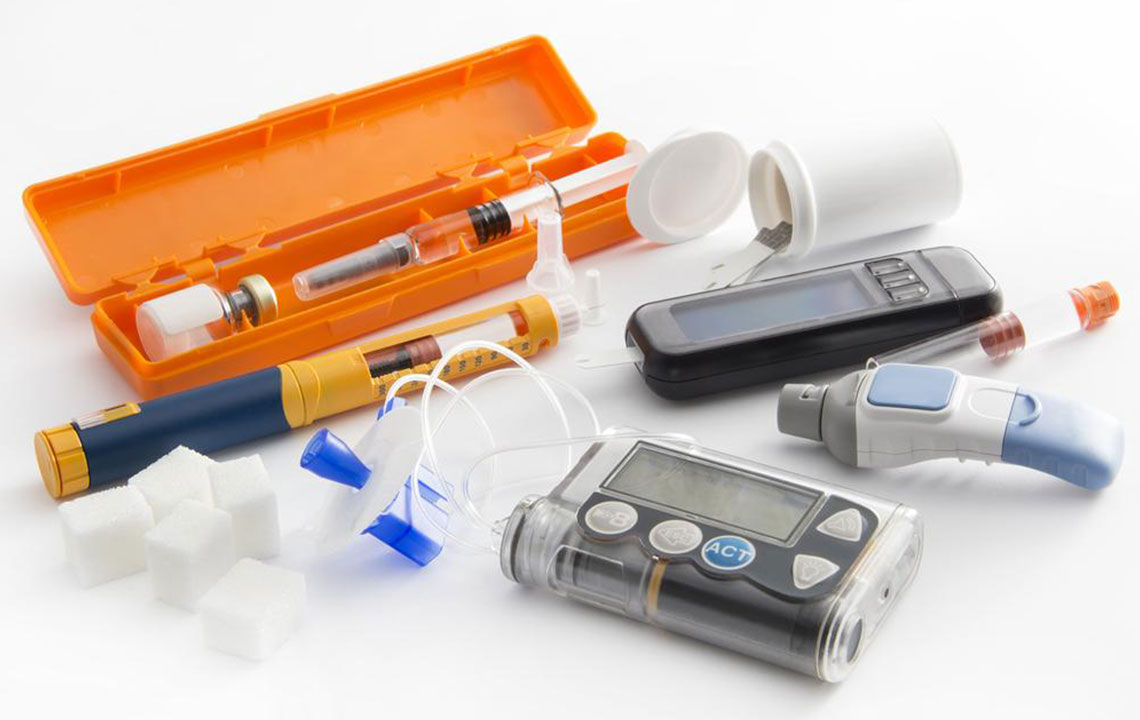
Medications and insulin therapy often become necessary when diet changes and physical activity alone do not maintain blood sugar within the desired ranges. Treatment plans are individualized, depending on factors like age, weight, blood sugar levels, and overall health. Doctors may prescribe various drugs or combinations to target different aspects of glucose regulation, including oral hypoglycemics, injectable medications, and insulin.
Medical interventions for type 2 diabetes include:
Insulin therapy
In recent years, insulin treatment has shifted toward earlier intervention for many patients, rather than reserving it for advanced stages of the disease. Since oral insulin is not feasible, injectable insulin remains the primary option. Different types of insulin—such as long-acting (detemir, glargine), rapid-acting (lispro, aspart), and intermediate-acting (isophane)—are used based on individual needs. Most patients begin with a basal (long-acting) insulin dose at night, with adjustments made over time to optimize blood glucose control throughout the day.
Bariatric surgery
For individuals with obesity and a BMI over 35, bariatric surgery has emerged as an effective treatment option. Studies indicate that between 55% and 95% of patients experience significant improvement, with many achieving normal blood glucose levels post-operation. This approach not only promotes weight loss but also helps in dramatically improving glycemic control and reducing reliance on medications. Surgery is typically considered when lifestyle modifications and medications fail to produce adequate results and when the patient's health risks justify the intervention.