Comprehensive Guide to the Five Major Types of Psoriasis and Their Impact on Skin Health
This comprehensive article delves into the five main types of psoriasis, explaining their unique features, affected areas, symptoms, and treatment options. It aims to educate readers about the diverse manifestations of psoriasis to foster better understanding, diagnosis, and management of this chronic skin condition for improved quality of life.

Comprehensive Guide to the Five Major Types of Psoriasis and Their Impact on Skin Health
Psoriasis is a chronic, non-contagious skin condition that affects millions of people worldwide. This autoimmune disorder causes the body's immune system to mistakenly attack healthy skin cells, resulting in rapid cell turnover and persistent skin inflammation. The hallmark of psoriasis is the development of thickened, scaly patches on various parts of the body, which can vary greatly in appearance, size, and severity. Understanding the different variants of psoriasis is crucial for accurate diagnosis, effective treatment, and managing the emotional and physical impacts of the disease. There are five primary types of psoriasis, each distinguished by specific features and areas affected, making it essential for patients and healthcare providers to recognize these differences for optimal care.
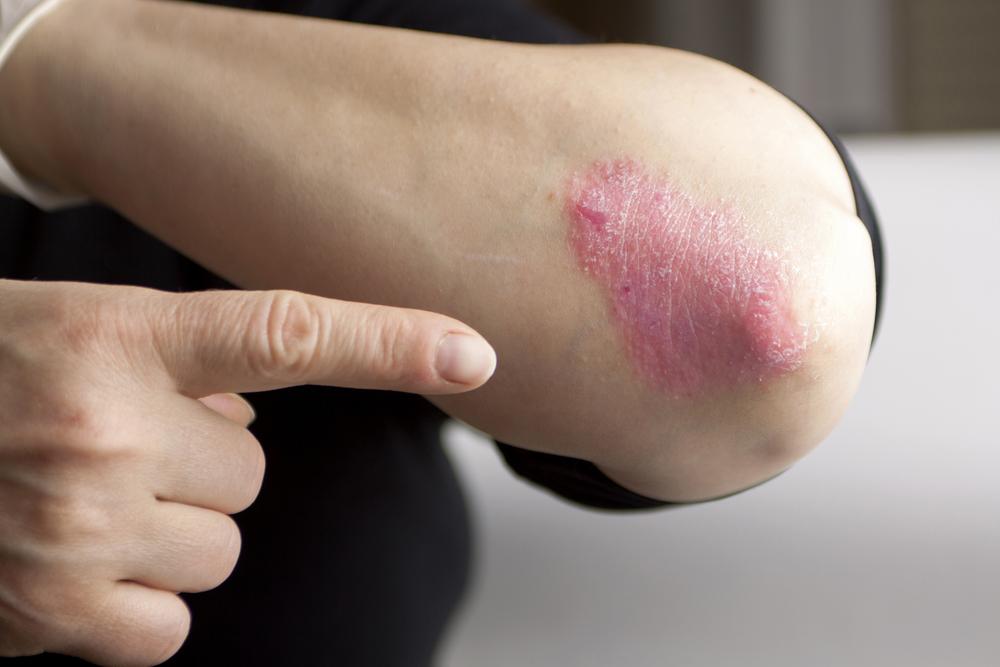
Plaque Psoriasis
This is the most common form of psoriasis, accounting for approximately 80% of all cases. It is characterized by raised, red patches of skin covered with silvery-white scales, often referred to as plaques. These plaques typically appear on accessible areas such as the elbows, knees, scalp, and lower back, but can occur anywhere on the body. The severity can range from minor patches to extensive, thickened areas that can cause significant discomfort. Plaque psoriasis tends to be persistent, fluctuating with periods of flare-ups and remission. It often impacts the patient's quality of life by causing itching, burning sensations, and emotional distress due to visible skin lesions.
Guttate Psoriasis
Guttate psoriasis is a distinct subtype that typically manifests as numerous small, drop-shaped red spots scattered across the skin. The name 'guttate' derives from the Latin word for 'drop.' These lesions are usually less than a centimeter in diameter and may appear suddenly, often following infections like strep throat or other respiratory illnesses. It commonly affects young adults and children, with lesions primarily present on the face, scalp, arms, legs, and trunk. Stress and illness can trigger or exacerbate guttate psoriasis. Though it might resemble an allergic rash or other skin conditions, proper diagnosis is key since guttate psoriasis can sometimes progress into plaque psoriasis if left untreated. Patients often experience mild to moderate itching, and the condition may resolve spontaneously within a few weeks or months with appropriate medical intervention.
Inverse Psoriasis
Also termed flexural psoriasis, inverse psoriasis affects skin folds and areas where the skin covers or creases, such as underarms, beneath the breasts, the groin, and around the buttocks. Unlike plaque psoriasis, the lesions in this form are less scaly but present as smooth, shiny, and inflamed patches that can be intensely itchy and painful. The moist environment of skin folds can worsen symptoms, especially with sweating, friction, or trapped dirt, leading to secondary bacterial or fungal infections. Inverse psoriasis often coexists with other forms of psoriasis and psoriasis-associated conditions like obesity or metabolic syndrome. Management involves a combination of topical therapies, moisture retention, and sometimes systemic treatments for severe or resistant cases. Patients often report significant discomfort and emotional distress due to the visibility and sensitivity of affected areas.
Pustular Psoriasis
Pustular psoriasis is a more severe and less common form, affecting roughly 3% of individuals with psoriasis. It is characterized by the presence of white pustules—small, non-infectious blisters filled with sterile pus—on inflamed skin. These pustules may be surrounded by areas of redness and swelling. Pustular psoriasis can manifest locally, often on the palms and soles (palmar-plantar pustulosis), or in a widespread manner across large parts of the body. Symptoms can include intense itching, burning pain, fever, chills, and malaise, especially during acute episodes. This form of psoriasis requires prompt medical attention to prevent complications. Triggers can include infections, stress, certain medications, or abrupt withdrawal of systemic treatments. Management involves topical corticosteroids, systemic medications like retinoids or immunosuppressants, and sometimes phototherapy. Given its severity, pustular psoriasis significantly impacts sufferers' daily routines and quality of life.
Erythrodermic Psoriasis
Erythrodermic psoriasis is an exceptionally rare but life-threatening form of the disease, affecting approximately 2% of psoriasis patients. It involves widespread redness, scaling, and shedding of the skin across most or all of the body surface. This extensive inflammation can compromise the skin’s barrier function, leading to dehydration, infections, and electrolyte imbalances. Symptoms include intense redness (erythema), swelling, warmth, severe itching, and pain. Patients often experience systemic symptoms like fever, chills, fatigue, and malaise. Erythrodermic psoriasis can develop suddenly or from a pre-existing psoriasis flare, especially if treatments are stopped abruptly or inadequately managed. Immediate hospitalization and intensive medical care are vital to address dehydration, prevent infections, and control inflammation. Treatment involves hospitalization, systemic immunosuppressants, corticosteroids, and supportive care. The condition poses a serious health risk and requires ongoing dermatological management to prevent recurrence and complications.
In conclusion, psoriasis exhibits a complex spectrum of clinical presentations, making individualized diagnosis and treatment essential. Patients should seek comprehensive evaluation from dermatologists to identify the specific variant affecting them. Advances in dermatology have led to more targeted therapies, improving outcomes and quality of life for those living with this chronic skin disorder. Awareness and understanding of these variants enable better management strategies, reduce stigma, and promote healthier skin and well-being.