Ultimate Comprehensive Guide to Psoriasis: Types, Symptoms, and Management Strategies
This comprehensive guide explores the various types of psoriasis, including plaque, guttate, inverse, nail, pustular, and erythrodermic. It details their symptoms, triggers, and treatment options, emphasizing the importance of professional diagnosis and personalized management strategies to improve quality of life. Whether dealing with mild or severe psoriasis, understanding these variants helps patients seek appropriate care and effective relief.

An in-depth exploration of Psoriasis: Variants, Characteristics, and Treatment Approaches
Psoriasis is a well-known chronic autoimmune skin condition that affects millions worldwide. Characterized by the development of abnormal skin patches, this disorder manifests as itchy, flaky, and often uncomfortable lesions that can appear on various parts of the body. Although its exact origins remain somewhat elusive, scientific research suggests that psoriasis involves an overactive immune response leading to accelerated skin cell production. Understanding the different types of psoriasis, their symptoms, triggers, and management options is essential for effective treatment and improved quality of life.
Exploring the Different Types of Psoriasis
Psoriasis is not a singular disease but a group of related conditions, each with unique features and implications. Identifying the specific type in an individual case helps tailor the most effective treatment plan.
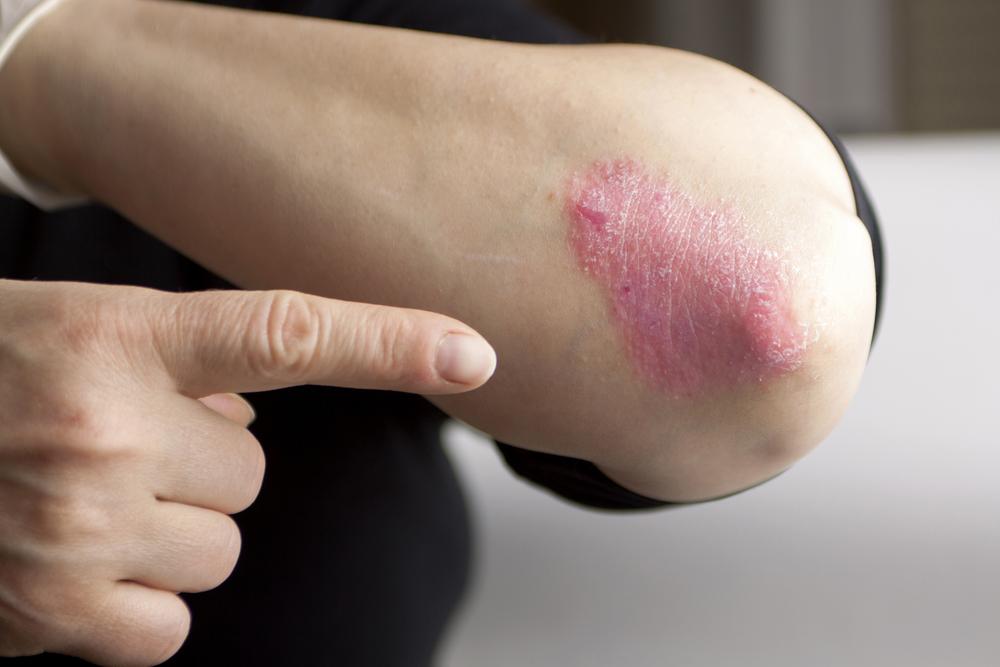
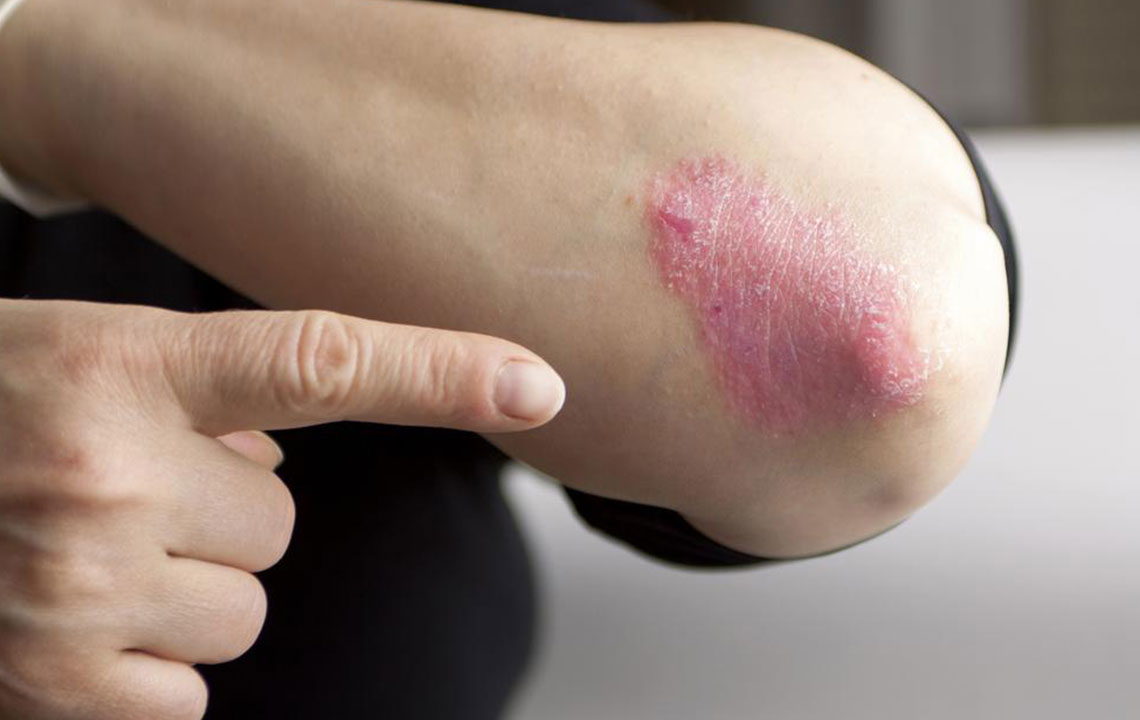
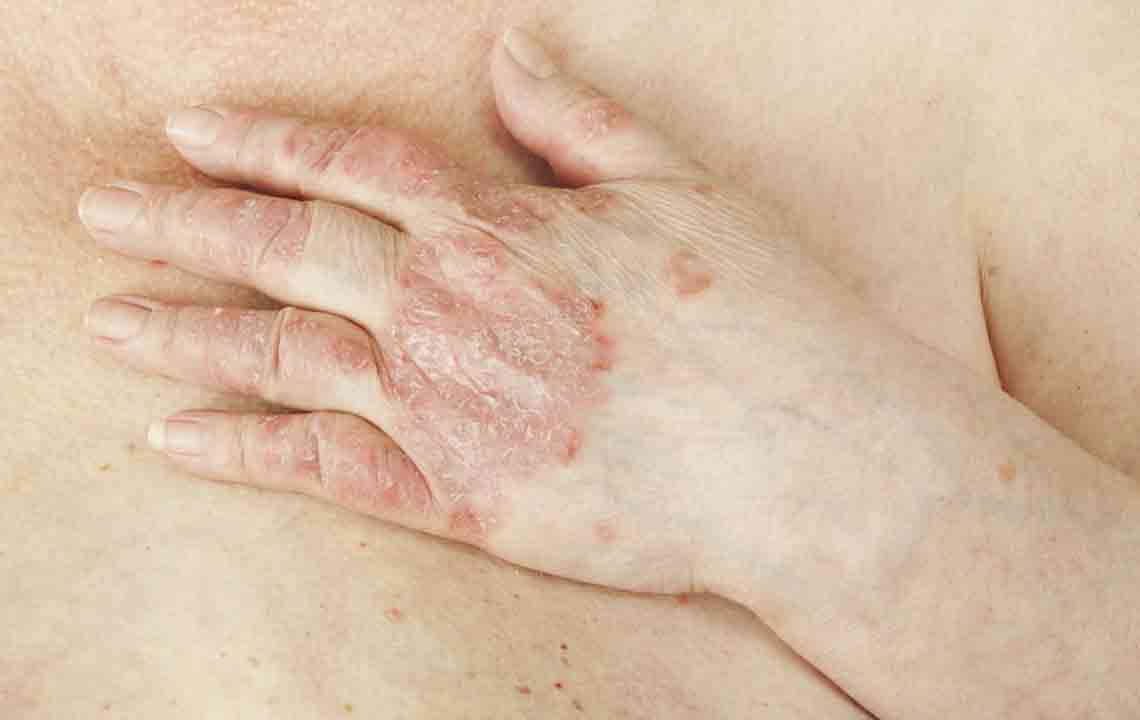
1. Plaque Psoriasis (Psoriasis Vulgaris)
This is the most prevalent form, accounting for approximately 80-90% of psoriasis cases. It is characterized by raised, inflamed, silvery-white scaly patches called plaques. These patches often appear on parts of the body where there is frequent skin friction or trauma, such as elbows, knees, lower back, and scalp. In more severe instances, plaques can spread extensively, involving areas like the face, hands, feet, genitals, and legs.
The plaques result from rapid proliferation of skin cells, which accumulate faster than they can shed, creating thickened patches. They are usually itchy, sometimes painful, and prone to cracking and bleeding. External triggers like stress, skin injuries, certain medications, infections, or environmental factors such as sun damage and cold weather can provoke flare-ups, though the precise cause remains unidentified. Genetic predisposition also plays a crucial role in the development of plaque psoriasis.
2. Guttate Psoriasis
This type primarily affects young adults and children. Often triggered by bacterial infections like streptococcal pharyngitis (strep throat), guttate psoriasis may appear suddenly and involve multiple small, drop-shaped lesions. These red or pink spots are usually less than 1 centimeter in diameter, tender, and may be itchy. They typically appear on the trunk, limbs, and legs, creating a scattered or widespread pattern. Stress, viral infections, or injuries can also serve as precipitating factors.
Management focuses on treating the underlying infection and controlling skin inflammation, often with topical therapies, phototherapy, or medications prescribed by healthcare providers.
3. Inverse Psoriasis
This variant develops in areas where skin folds and friction are frequent, such as the armpits, under the breasts, groin, or around the genitals and buttocks. Unlike other psoriasis types, inverse psoriasis presents as shiny, smooth, and red patches without significant scaling due to moisture levels in these areas. Symptoms include soreness, burning, and itching, often worsened by sweating and friction. Warm, moist environments foster fungal infections, which can complicate diagnosis and treatment.
Patients may experience secondary bacterial infections, leading to pus-filled bumps, foul odors, swelling, and tenderness. Management involves anti-inflammatory treatments, antifungal medications if necessary, and proper hygiene practices to reduce friction and moisture buildup.
4. Nail Psoriasis
Nail involvement occurs in approximately 50% of psoriasis cases and can serve as a diagnostic clue. Affected nails often show discoloration, pitting, ridging, or crumbling, similar to fungal infections but distinguishable by their pattern and associated skin findings. Discolorations may appear as yellow, red, or brown spots, and nails can become thickened, brittle, and prone to detachment.
Loss of nail luster, grooves, and abnormal growth are common signs. Nail psoriasis significantly impacts quality of life, especially when it affects fingernails, affecting daily activities and self-esteem. It is more common in individuals over 40 but can occur at any age. Treatment options include topical corticosteroids, vitamin D analogs, systemic therapies, and biologics for severe cases.
5. Pustular Psoriasis
This less common but more severe subtype involves the formation of white, pus-filled blisters (pustules) on red, inflamed skin. It may appear as localized pustules on the hands and feet or as widespread pustular psoriasis affecting larger skin areas. When generalized, symptoms can include fever, chills, fatigue, and malaise, reflecting systemic involvement.
Variants like palmoplantar pustulosis (affecting palms and soles) and Achrodermatitis continua of Hallopeau (affecting fingertips) are notable. Treatment strategies often involve potent topical steroids, phototherapy, systemic immunosuppressants, and biologic agents to suppress immune activity.
6. Erythrodermic Psoriasis
The most severe and rare form, erythrodermic psoriasis, results in widespread redness, scaling, and skin exfoliation over large body surface areas. It often arises from the worsening of existing psoriasis or from uncontrolled disease, sometimes triggered by abrupt withdrawal of systemic medications or infections.
Patients experience severe discomfort, dehydration, electrolyte imbalance, fever, chills, and rapid heartbeat. The skin becomes fragile and vulnerable to infections. This condition demands urgent medical intervention, often hospitalization with intensive treatment involving systemic medications, fluids, and wound care.
Recognizing Common Psoriasis Symptoms
While each type has distinct features, typical symptoms across all variants include thickened, red, and inflamed skin covered with silvery or white scales. Patients frequently report itching, burning sensations, skin cracking, bleeding, and discomfort. Nail changes, such as pits and discoloration, are also common. Sleep disturbances may occur due to discomfort, and emotional distress is a significant concern for many individuals.
Diagnosing psoriasis should always be performed by a healthcare professional. Visual examination, patient history, and sometimes skin biopsies are employed for accurate diagnosis, as many skin conditions mimic psoriasis.
Managing and Treating Psoriasis
While there is currently no cure for psoriasis, numerous treatment options exist tailored to the specific type and severity of the condition. Lifestyle modifications, including stress reduction, avoiding triggers, maintaining skin moisture, and adopting a balanced diet, can significantly impact disease control.
Medical treatments range from topical therapies like corticosteroids, vitamin D analogs, moisturizers, and coal tar preparations to phototherapy (UVB light treatment). In moderate to severe cases, systemic medications such as methotrexate, cyclosporine, or retinoids are prescribed. The advent of biologic therapies targeting specific immune pathways has revolutionized psoriasis management, offering hope for remission in many cases.
Regular follow-up with healthcare providers is essential to monitor treatment efficacy and side effects, especially when systemic or biologic agents are used. Patients are also encouraged to join support groups and seek counseling to cope with the psychological impacts associated with psoriasis.