Effective Strategies for Managing and Treating Dry Eye Syndrome
Dry eye syndrome affects millions globally, especially middle-aged and elderly individuals. Effective management involves targeted eye drops, lifestyle changes, and professional treatment. Recognizing causes such as aging, environmental factors, and medication use can help tailor effective solutions, including artificial tears and prescription medications. Consulting an eye specialist is crucial for personalized care, helping restore comfort and protect eye health. This comprehensive approach ensures relief from symptoms and preserves vision, significantly enhancing patients' quality of life. Implementing proper treatment plans is vital for long-term eye health preservation.

Effective Strategies for Managing and Treating Dry Eye Syndrome
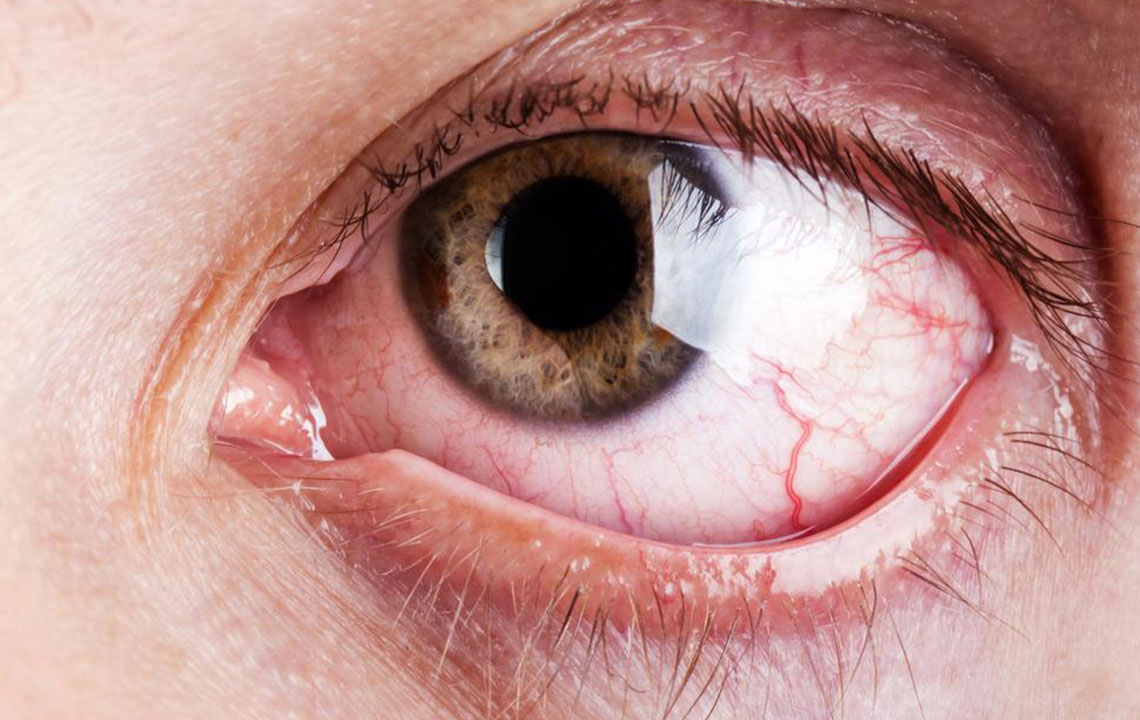
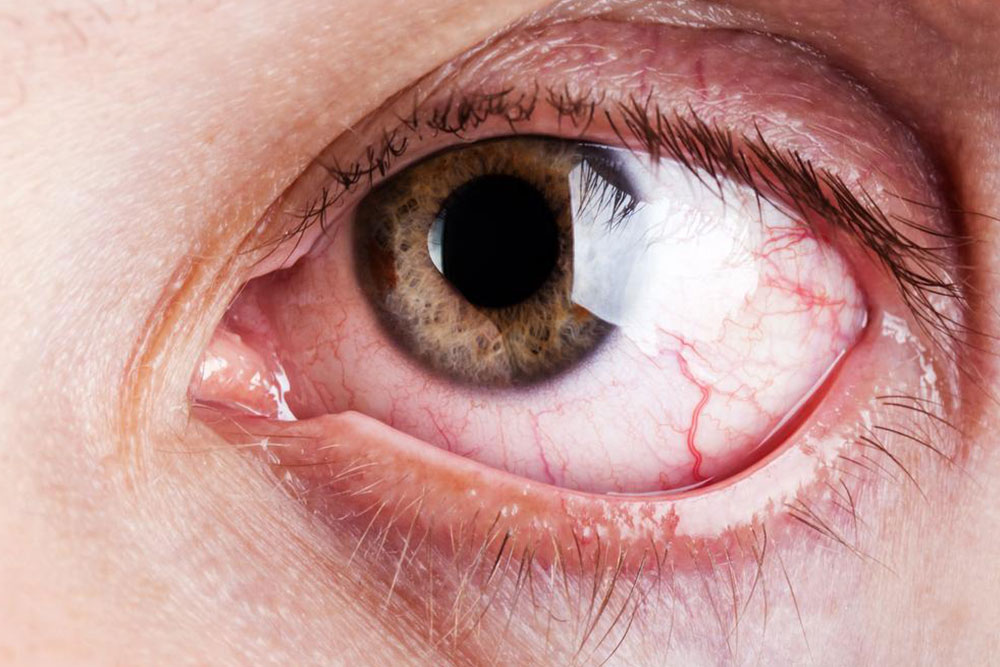
Dry eye syndrome, medically known as keratoconjunctivitis sicca, is a prevalent ocular condition that affects millions worldwide, particularly in middle-aged and elderly populations. This condition occurs when the eyes do not produce enough tears or when the tears evaporate too quickly, leading to dryness, discomfort, and potential damage to the eye surface. The impact of dry eye syndrome extends beyond mere discomfort, as it can interfere with daily activities like reading, computer work, and driving, significantly affecting quality of life. Understanding the causes, symptoms, and available treatment options is crucial for effective management.
In modern society, dry eye syndrome has become increasingly common due to various environmental and lifestyle factors. Factors such as prolonged exposure to digital screens, air conditioning, pollution, and irritants contribute significantly to tear film instability. Ageing is also a major risk factor, as tear production tends to decrease over time. Hormonal fluctuations, especially in women during pregnancy, menopause, or use of contraceptives, further exacerbate the condition. Additionally, certain medications, like antihistamines, antidepressants, and blood pressure medications, can reduce tear production leading to dry eye symptoms.
Effectively diagnosing and treating dry eye syndrome involves a comprehensive approach. A visit to an eye care professional can determine the severity and the underlying causes, guiding personalized treatment strategies. Today, a myriad of therapies are available, ranging from simple eye drops to advanced medical procedures. Many patients find relief through topical treatments, lifestyle modifications, and in some cases, surgical interventions. It’s important to recognize that treating dry eyes not only alleviates discomfort but also protects the integrity of the ocular surface, preventing chronic damage.
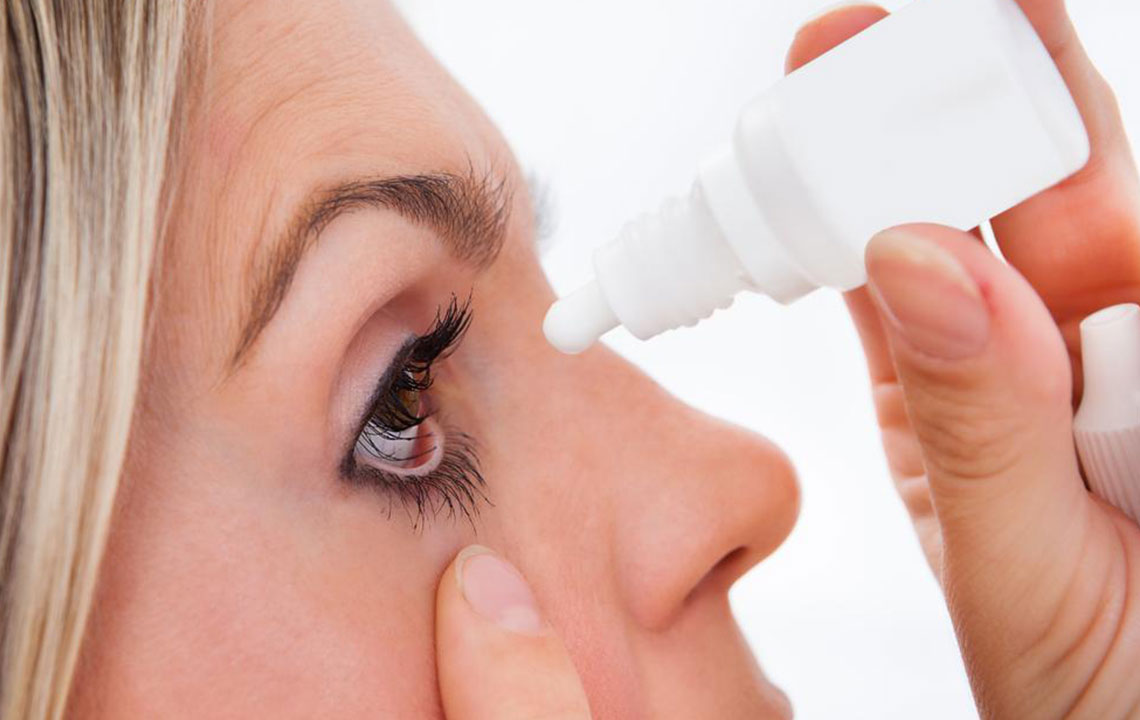
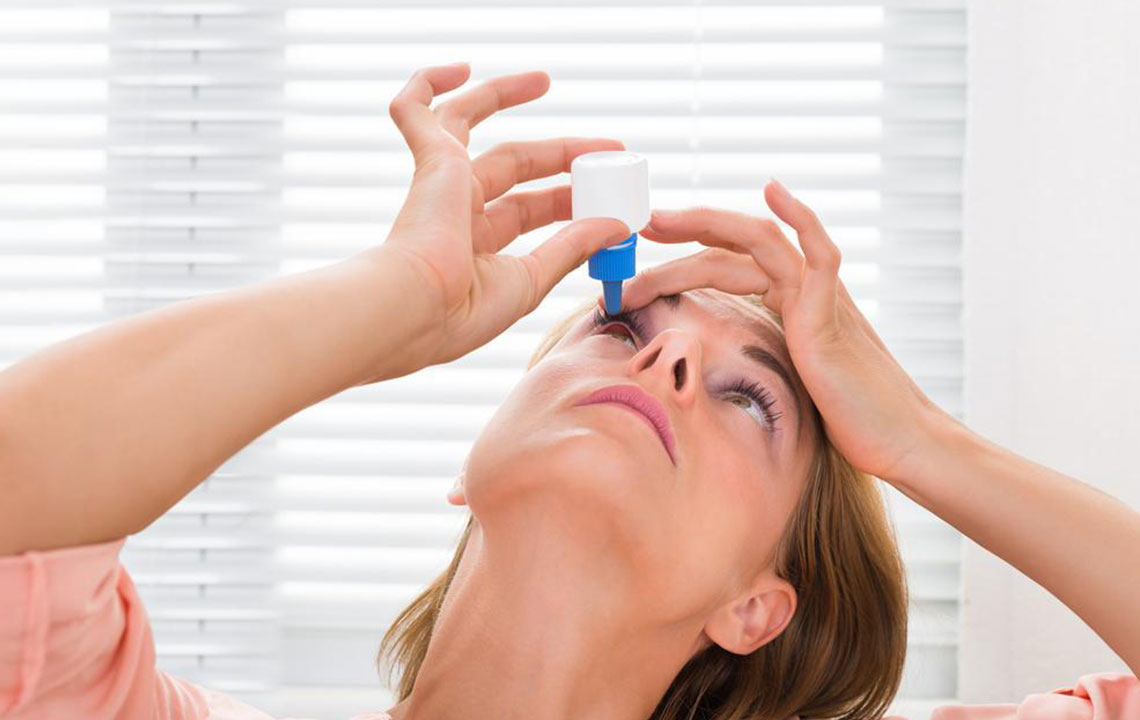
Among the most common and effective treatments are various types of eye drops. These solutions are tailored to replenish moisture, reduce inflammation, and stimulate tear production. Choosing the right eye drop depends on individual needs and underlying causes, which a healthcare professional can recommend. Here are some of the most widely used treatments:
Artificial tears: The cornerstone of dry eye treatment, these lubricating drops help hydrate the eyes and provide immediate relief from dryness and irritation. It’s important to select formulas that are preservative-free if used frequently, especially for sensitive eyes.
Cyclosporine eye drops: An immunomodulatory medication that boosts natural tear production by reducing inflammation of the lachrymal glands. These require a prescription and are typically used twice daily for best results.
Lifitegrast: This prescription eye drop targets inflammation by inhibiting T-cell activity, often used in moderate to severe dry eye cases.
Autologous serum drops: Made from the patient’s own blood, these drops are used in severe or refractory cases where conventional treatments are insufficient. They provide nutrients and healing factors to the ocular surface.
Additional care: Lifestyle changes such as increasing humidification in living spaces, avoiding smoke and wind exposure, and practicing proper blinking techniques can significantly support treatment outcomes. Omega-3 fatty acid supplements are also beneficial in improving tear quality.
Before initiating any treatment, consider these essential guidelines:
Always consult with an eye care specialist to determine the most appropriate therapy based on your specific condition.
Avoid using eye drops formulated solely for redness reduction, as they can worsen dryness with prolonged use.
If you have pre-existing eye conditions such as glaucoma or ocular allergies, seek professional advice to avoid adverse interactions.
Understand that ingredients differ among products; what is effective for one person may not work for another.
Opt for preservative-free formulations if you have sensitive eyes or need frequent application, to minimize irritation.
Understanding the causes of dry eyes
Environmental factors like dust, wind, dry air, pollution, and screen exposure are primary contributors.
Chronic dry eye can result from underlying health conditions such as autoimmune diseases (e.g., Sjögren’s syndrome), thyroid disorders, or diabetes.
Medications like antihistamines, antidepressants, and medications for high blood pressure can impair tear production.
Aging naturally decreases tear film stability and production, making age a significant risk factor.
Prolonged use of digital devices without breaks, exposure to air conditioning or heating systems, and living in dry climates also heighten risk.
In summary, managing dry eye syndrome requires a combination of medical treatment, lifestyle modifications, and ongoing monitoring. While the condition may be common, effective interventions exist to restore comfort and preserve eye health. Awareness and early intervention are key to preventing complications and improving quality of life for those affected by this persistent condition.