Comprehensive Guide to Rheumatoid Arthritis: Recognizing Symptoms and Exploring Treatment Strategies
This detailed guide covers rheumatoid arthritis, including its symptoms, diagnosis, and a range of treatment strategies from medications to surgery. Recognizing early signs is key to preventing joint damage and managing a chronic autoimmune condition effectively. The article emphasizes a multidisciplinary approach to treatment, highlighting lifestyle adjustments and advanced therapies that improve quality of life for RA patients.
Comprehensive Guide to Rheumatoid Arthritis: Recognizing Symptoms and Exploring Treatment Strategies
Rheumatoid arthritis (RA) is a chronic, progressive autoimmune disorder that primarily affects the joints but can also impact other organs and systems within the body. It is characterized by an abnormal immune response where the immune system mistakenly attacks healthy joint tissues, leading to inflammation, pain, swelling, and eventual joint damage. Understanding the nuances of RA, including its symptoms, progression, and available treatment options, is essential for early intervention, effective management, and improving quality of life for those affected. This comprehensive guide aims to shed light on the complex nature of rheumatoid arthritis while offering insights into current medical approaches, lifestyle adaptations, and surgical interventions.
Understanding Rheumatoid Arthritis: An In-Depth Overview
Rheumatoid arthritis is a systemic autoimmune disease with a multifaceted pathology. Unlike osteoarthritis, which results from wear and tear, RA stems from immune-mediated attack on synovial tissues, leading to synovitis and joint destruction. The exact cause remains unknown, but genetic, environmental, and hormonal factors are known to influence susceptibility. Notably, RA can manifest at any age but most commonly affects individuals between 30 and 60 years old, with women being disproportionately affected. Early diagnosis and management are crucial in preventing irreversible joint damage.
The disease progression typically involves stages, starting with mild synovial inflammation, which can escalate to severe joint deformities if left untreated. RA often follows periods of flare-ups and remission, with symptoms fluctuating in intensity. Over time, persistent inflammation can cause cartilage destruction, bone erosion, and deformities, severely impairing joint function and mobility. Beyond joints, RA may lead to systemic complications, including cardiovascular disease, lung involvement, and eye inflammation, emphasizing its potential to impact overall health.
Recognizing the Symptoms of Rheumatoid Arthritis
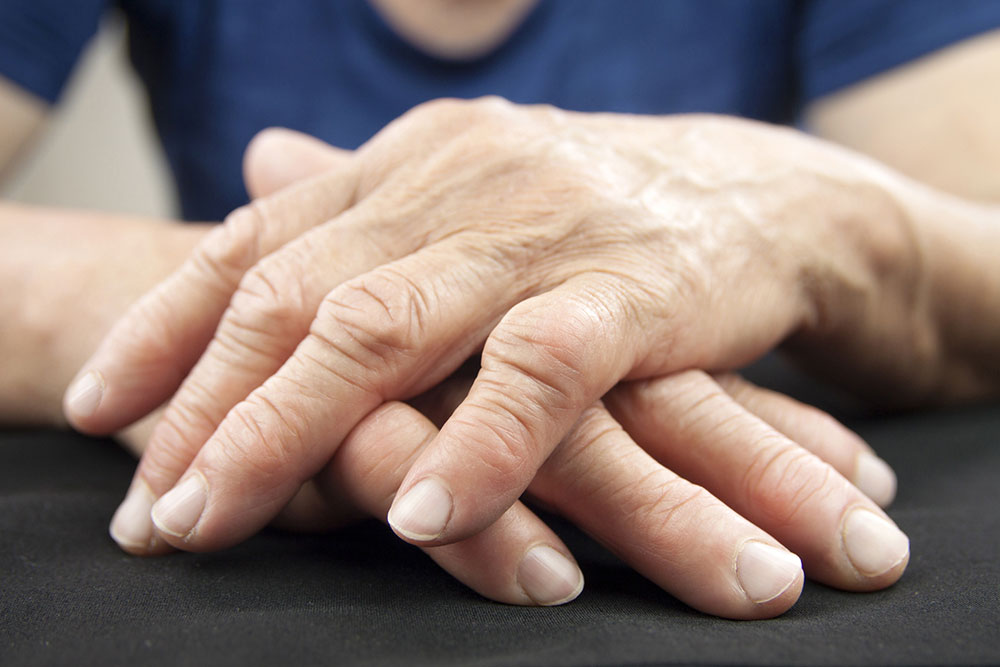
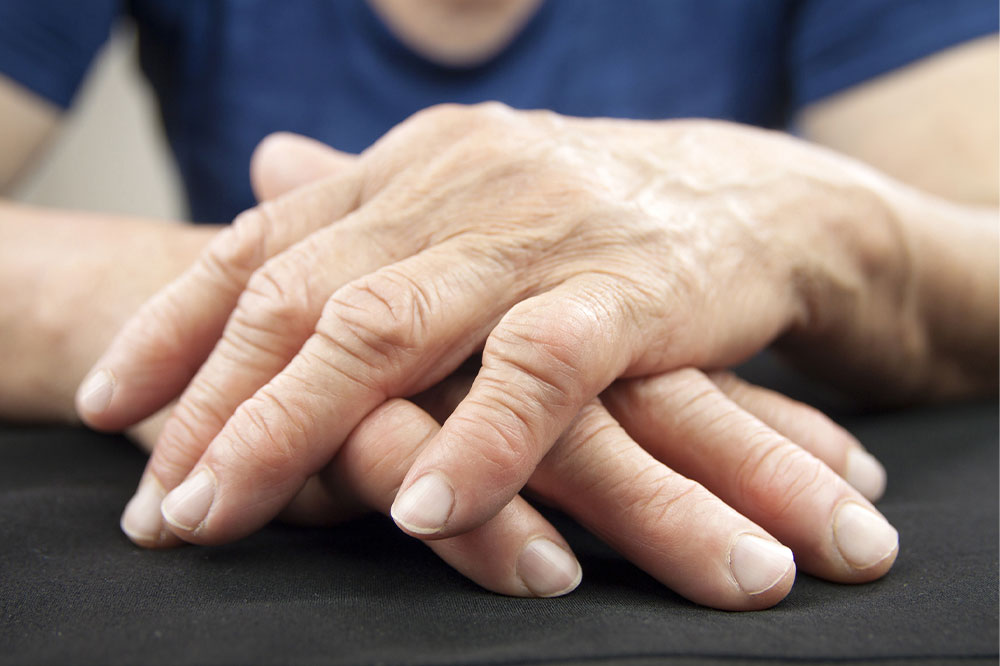
Symptoms of RA vary widely among individuals and may evolve over time. Awareness of early signs can facilitate prompt intervention, reducing the risk of permanent damage. Some of the most common symptoms include:
Limping or difficulty walking due to joint pain or deformity
Persistent fatigue and exhaustion
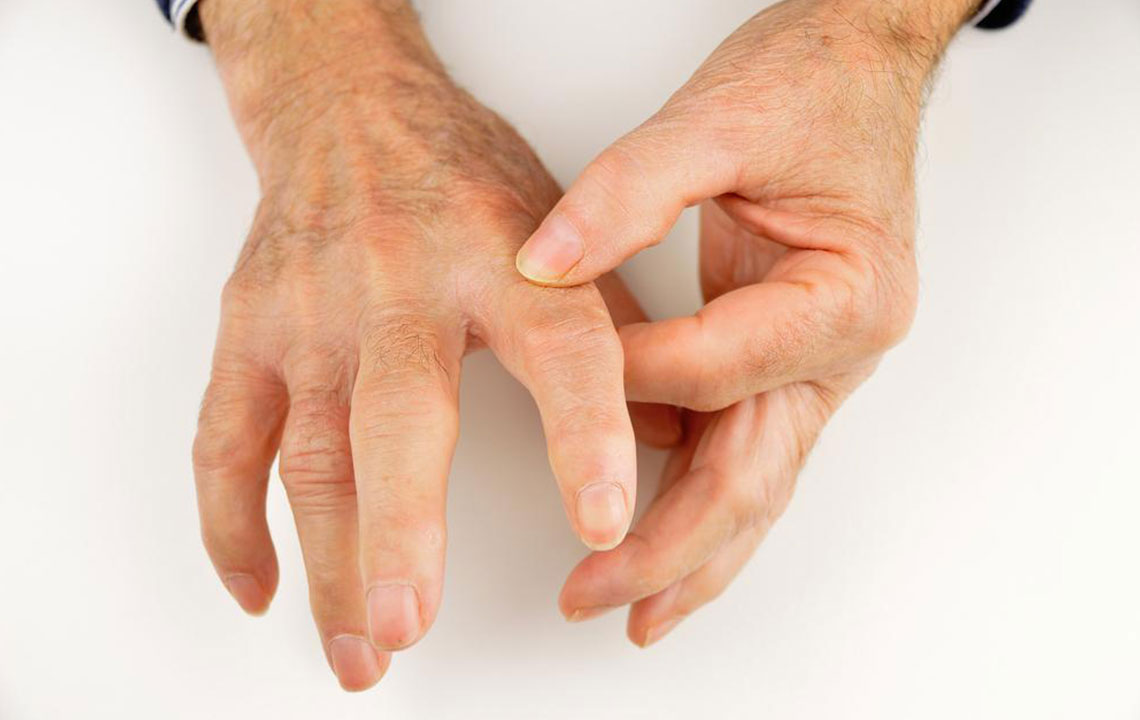
Swelling and tenderness in multiple joints
Prolonged joint stiffness, especially in the morning (lasting more than an hour)
Redness and warmth around affected joints
Fever and general malaise during flare-ups
Symptoms of anemia such as pallor and weakness
Decreased range of motion and joint instability
Visible joint deformities in advanced stages
Multiple joint involvement, often symmetrically affecting hands, wrists, elbows, knees, and ankles
In addition to joint-related symptoms, RA may manifest systemic features like nodules under the skin, lung inflammation, and vasculitis, further complicating the clinical picture.
Diagnostic Strategies for Rheumatoid Arthritis
Diagnosing RA involves a combination of clinical evaluation, laboratory testing, and imaging studies. Rheumatologists consider the pattern and duration of symptoms, physical examination findings, and serological markers to confirm the diagnosis.
Blood tests: Rheumatoid factor (RF), anti-citrullinated protein antibodies (ACPA), elevated erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP) levels indicate inflammation and autoimmune activity.
Imaging: X-rays, ultrasound, and MRI scans can reveal joint erosion, cartilage loss, and synovial swelling, helping monitor disease progression.
Early diagnosis enables timely initiation of interventions that can reduce joint damage and improve long-term outcomes.
Current Treatment Options for Rheumatoid Arthritis
While there is no cure for RA, numerous treatment strategies aim to control symptoms, suppress immune overactivity, and prevent joint destruction. The choice of therapy depends on disease severity, progression, and individual patient factors. A multidisciplinary approach involving rheumatologists, physical therapists, and other healthcare providers provides the best chance for effective management.
Pharmacological Interventions
NSAIDs: Nonsteroidal anti-inflammatory drugs such as ibuprofen, naproxen, and diclofenac are often first-line agents to alleviate pain and reduce inflammation. While effective, they require cautious use to avoid gastrointestinal, cardiovascular, liver, and kidney side effects.
DMARDs (Disease-Modifying Antirheumatic Drugs): These are cornerstone medications that alter the disease course. Methotrexate remains the most widely prescribed DMARD, effectively reducing joint damage. Other options include sulfasalazine, hydroxychloroquine, and leflunomide. These drugs may have side effects like bone marrow suppression, liver toxicity, and gastrointestinal disturbances, necessitating regular monitoring.
Corticosteroids: Prednisone and methylprednisolone are used for rapid symptom relief during flare-ups. Long-term use is limited by side effects like osteoporosis, weight gain, and increased infection risk.
Biologic Agents: Targeted therapies such as adalimumab, infliximab, etanercept, and rituximab have revolutionized RA treatment by inhibiting specific immune components involved in inflammation. These drugs are often reserved for moderate to severe disease refractory to conventional therapies and require careful screening due to infection risks.
Combining these medications forms a personalized treatment plan aimed at disease remission or low disease activity.
Non-Pharmacological and Supportive Therapies
Complementary to medication, lifestyle modifications and supportive therapies are essential components of comprehensive RA management. These include:
Engaging in joint-friendly exercises like swimming or physiotherapy to maintain flexibility and muscle strength.
Occupational therapy to adapt daily activities and reduce joint stress, including the use of ergonomic devices and assistive tools.
Pain management strategies, including heat and cold therapy, acupuncture, or transcutaneous electrical nerve stimulation (TENS).
Dietary modifications emphasizing anti-inflammatory nutrients and adequate nutrition support immune health.
Preventive measures against osteoporosis, such as calcium and vitamin D supplementation and bone density monitoring, especially when using corticosteroids.
Patient education and psychological support are vital for coping with chronic illness, enhancing adherence to treatment, and improving overall well-being.
Surgical Options for Advanced Rheumatoid Arthritis
When conservative therapies no longer suffice and joint damage becomes severe, surgical interventions may restore function and relieve pain. Common procedures include:
Joint Repair and Debridement: Removal of loose cartilage or inflammatory tissue to improve joint function in early damage stages.
Joint Fusion (Arthrodesis): Fusing bones to stabilize painful, deformed joints, often used in the wrists and ankles.
Joint Replacement (Arthroplasty): Replacing damaged joints with artificial prostheses, notably in hips and knees, to restore mobility and alleviate pain.
While these surgeries can significantly enhance quality of life, they carry risks such as infection, blood clots, and prosthesis complications. A thorough preoperative evaluation and postoperative rehabilitation are crucial.
In conclusion, managing rheumatoid arthritis requires a comprehensive understanding of its symptoms, progression, and treatment modalities. Advances in medical therapies, combined with lifestyle modifications and surgical options, have vastly improved patient outcomes. Early diagnosis and personalized care are essential for halting disease progression, preserving joint function, and maintaining an active, pain-free life.