Comprehensive Guide to Diabetic Peripheral Neuropathy: Causes, Symptoms, and Management
Diabetic peripheral neuropathy is a common complication of diabetes that damages nerves outside the central nervous system, especially in the feet and legs. This comprehensive guide explores its causes, symptoms, and effective strategies for management, emphasizing the importance of blood sugar control and preventive care to avoid severe complications such as ulcers and amputations. Regular monitoring, proper foot care, and advances in diagnostic tools are vital for early detection and treatment, enhancing patients' quality of life and minimizing long-term damage.

Understanding Diabetic Peripheral Neuropathy: Causes, Symptoms, and Effective Management
Diabetic peripheral neuropathy (DPN) is one of the most common and concerning complications faced by individuals living with diabetes. It involves damage to the peripheral nerves, which are responsible for transmitting signals between the central nervous system and the limbs, especially the feet and hands. This condition is primarily caused by prolonged high blood glucose levels, which damage small blood vessels and nerves, leading to a range of sensory and motor impairments.
As diabetes progresses, uncontrolled blood sugar can cause significant harm to small blood vessels that nourish the nerves. These blood vessels, known as microvasculature, are essential for maintaining nerve health and function. When these vessels become damaged, nerves do not receive enough oxygen and nutrients, leading to nerve fiber degeneration. Over time, this results in symptoms such as numbness, tingling, burning sensations, and muscle weakness, predominantly in the feet and legs, though the hands can also be affected.
Diabetic peripheral neuropathy is classified under several types, including distal symmetric polyneuropathy, which affects the longest nerves first, typically starting in the toes and progressing upward. Other types include autonomic neuropathy, which affects involuntary functions like blood pressure and digestion, and proximal neuropathy, causing weakness in the thighs and hips.
Understanding the risk factors that contribute to DPN is vital for prevention and management. Besides prolonged high blood glucose, factors such as hypertension, high cholesterol levels, smoking, and obesity exacerbate nerve damage. Genetic predisposition may also play a role in determining who develops neuropathy among diabetics. Early diagnosis and intervention can significantly reduce the risk of severe complications.
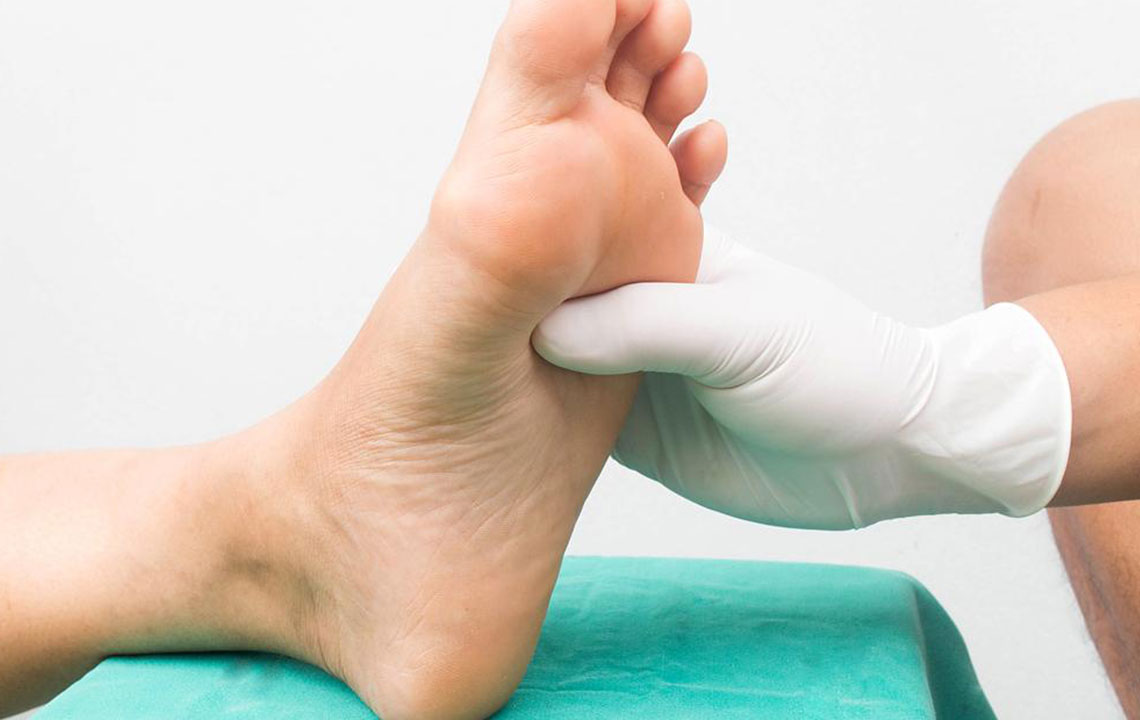
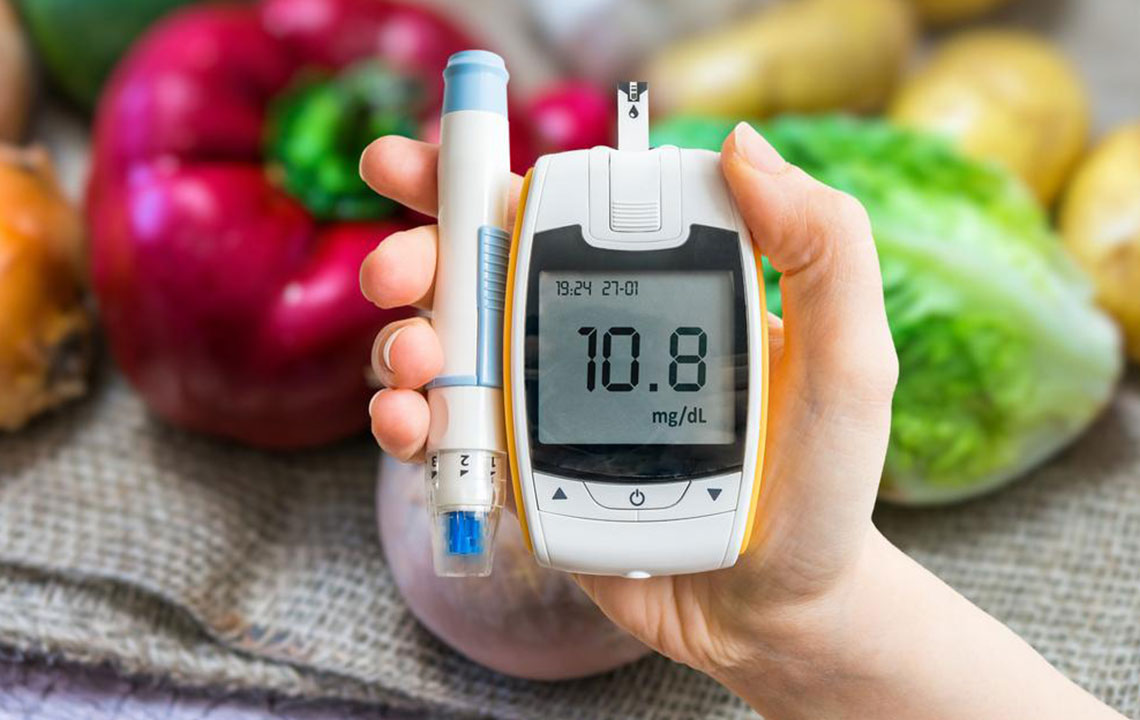
Since diabetic peripheral neuropathy is an incurable condition, the focus is ultimately on managing blood sugar levels to prevent or slow the progression of nerve damage. Effective blood glucose control involves a combination of medication adherence, dietary modifications, regular physical activity, and blood sugar monitoring. In addition, patients should undergo routine foot examinations to identify early signs of nerve damage and prevent complications like ulcers or infections which can necessitate amputations.
Recent advances in diagnostic technology have improved the detection and monitoring of peripheral nerve damage. Nerve conduction studies and electromyography (EMG) are used to measure nerve function, while skin biopsies help quantify nerve fiber loss. These tests assist clinicians in tailoring individualized treatment plans and tracking disease progression accurately.
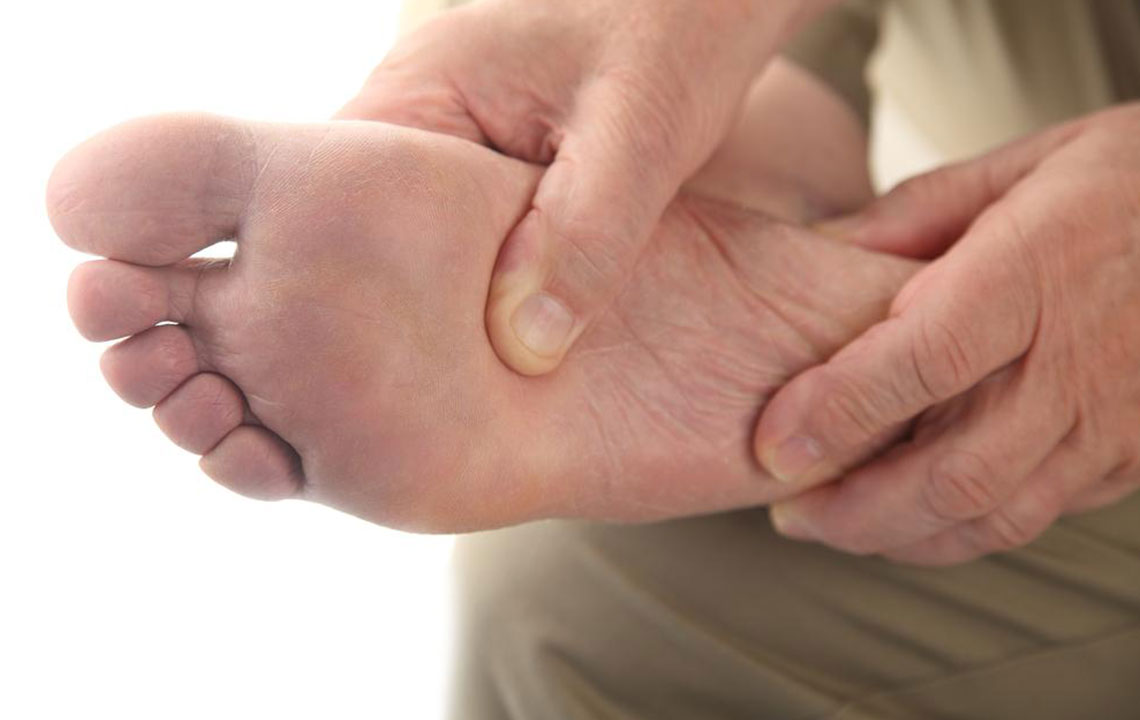
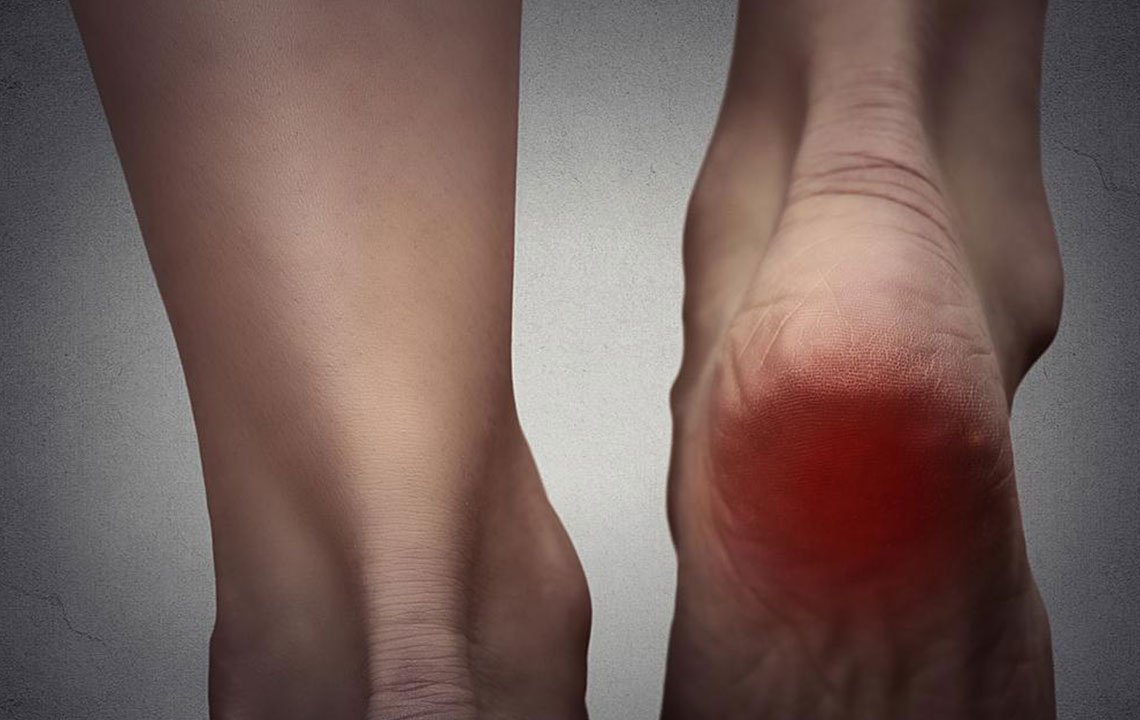
Symptoms of diabetic peripheral neuropathy can vary widely among patients, but common signs include numbness, tingling, burning sensations, and sharp pains, particularly in the feet and lower legs. As the condition advances, patients may experience a loss of sensation, making it difficult to detect injuries or burns, which increases the risk of infections and ulcers. Proper foot care is essential for individuals with diabetes, including daily inspections, wearing protective footwear, and avoiding walking barefoot.
Preventive measures such as custom footwear, orthotics, and nerve protection gloves are recommended to minimize injury risks. Additionally, managing other health conditions like hypertension and cholesterol also supports nerve health. Patients should focus on maintaining good glycemic control, which has been proven to slow the progression of neuropathy.
In cases where nerve pain becomes severe, medications such as anticonvulsants, antidepressants, and topical agents can provide relief. Physical therapy and occupational therapy are also valuable in improving strength and functionality. Lifestyle modifications, including quitting smoking and losing weight, further enhance overall nerve health and reduce the risk of complications.
Living with diabetic peripheral neuropathy requires ongoing management and education. Patients should be encouraged to adhere to their treatment plans, maintain regular medical checkups, and educate themselves about foot care and infection prevention. Support groups and diabetes education programs provide vital resources and motivation for those coping with this chronic condition.
Proper management of diabetic peripheral neuropathy is crucial for improving quality of life and preventing serious complications like foot ulcers and amputations. Through vigilant blood sugar control, routine screenings, and protective measures, individuals with diabetes can effectively manage this condition and preserve nerve function for as long as possible.