Comprehensive Guide to Rheumatoid Arthritis: Symptoms, Diagnosis, Treatment Options, and Lifestyle Management
Discover the comprehensive guide to rheumatoid arthritis, including its symptoms, diagnostic procedures, treatment options, and lifestyle tips. Understand how early intervention and personalized care can enhance quality of life despite this chronic autoimmune disease. Learn about medication therapies, lifestyle modifications, and when surgical options may be necessary to manage RA effectively.
Comprehensive Guide to Rheumatoid Arthritis: Symptoms, Diagnosis, Treatment Options, and Lifestyle Management
Rheumatoid arthritis (RA) is a complex, long-term autoimmune disorder that predominantly targets the joints, leading to chronic inflammation. This condition is characterized by pain, swelling, stiffness, and a progressive decline in joint function, which can significantly impair daily activities and quality of life. RA is not merely a joint disease; it can also affect various organ systems, making early diagnosis and comprehensive management essential for preventing severe complications. Understanding the underlying causes, recognizing early symptoms, and exploring effective treatment strategies are vital steps in managing this debilitating disease.
Rheumatoid arthritis affects millions worldwide, regardless of age, although it most commonly appears between ages 30 and 60. Women are at higher risk than men, which suggests hormonal and genetic factors may influence disease development. The disease stems from an abnormal immune response where the body's immune system mistakenly identifies joint tissues as foreign and attacks them, causing inflammation and tissue damage. Over time, this process can lead to joint deformity, loss of function, and decreased mobility if not properly treated.
Recognizing the Signs and Symptoms of Rheumatoid Arthritis
Early detection of RA is crucial for initiating treatment that can slow disease progression and reduce joint damage. Symptoms can vary widely among individuals, but typically include persistent joint pain, swelling, and stiffness, especially in the morning or after periods of inactivity. Symmetric joint involvement—meaning the same joints on both sides of the body are affected—is a hallmark feature of RA. Commonly affected joints include the fingers, wrists, knees, elbows, and shoulders.
In addition to joint symptoms, other signs may include fatigue, low-grade fever, loss of appetite, and general malaise. As the disease progresses, joint deformities and erosion can occur, leading to decreased range of motion and functional impairments. Some individuals may also develop extra-articular symptoms such as inflammation of the eyes, skin nodules, or lung involvement.
Diagnostic Approaches for Rheumatoid Arthritis
Diagnosing RA involves a combination of clinical assessment, laboratory tests, and imaging studies. Your healthcare provider will perform a thorough physical examination to check for joint swelling, tenderness, and deformities. Blood tests, such as rheumatoid factor (RF), anti-cyclic citrullinated peptide (anti-CCP) antibody, erythrocyte sedimentation rate (ESR), and C-reactive protein (CRP), help detect inflammation and autoimmune activity. Elevations in these markers can support an RA diagnosis, although they are not definitive on their own.
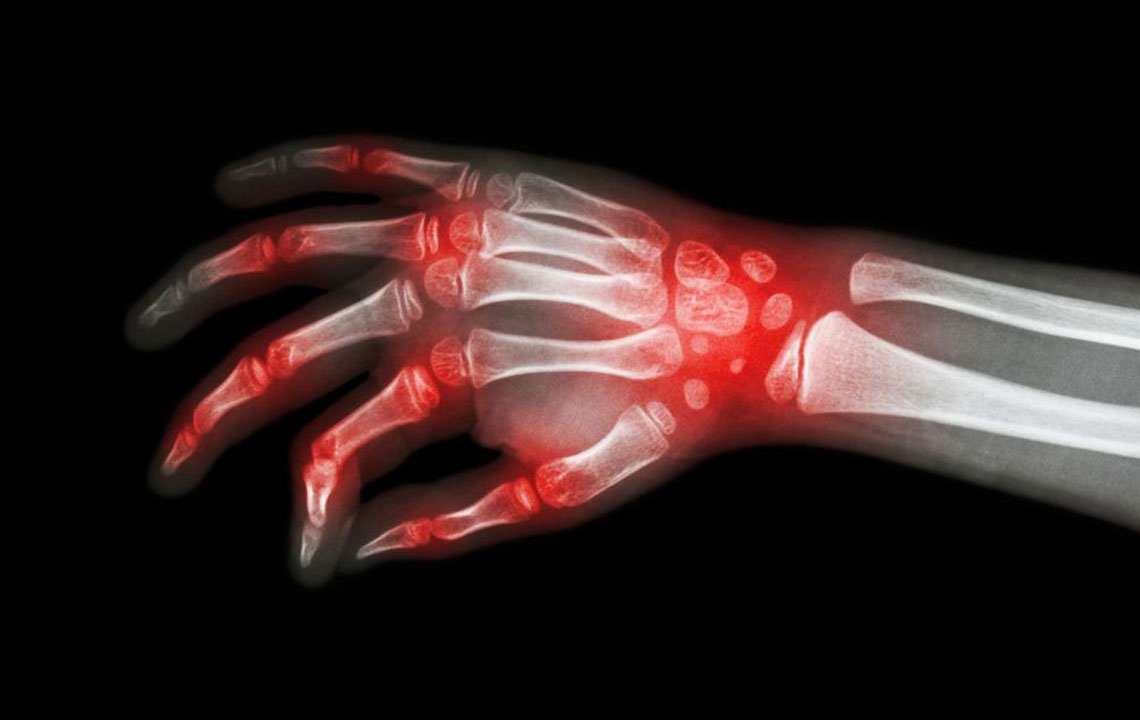
Imaging techniques like X-rays, ultrasounds, or MRI scans are essential for visualizing joint damage, monitoring disease progression, and guiding treatment decisions. Early imaging can reveal subtle changes before significant deformity develops. It is important for patients to keep detailed records of symptoms and any functional limitations to aid healthcare providers in forming accurate diagnoses and personalized treatment plans.
Life-Long Management of Rheumatoid Arthritis
Since RA is a chronic condition, effective management focuses on controlling inflammation, alleviating symptoms, preventing joint destruction, and maintaining quality of life. Treatment strategies are tailored to each individual based on symptom severity, disease progression, and overall health status. A multidisciplinary approach often yields the best results, incorporating medication use, lifestyle modifications, physical therapy, and sometimes surgical interventions.
Medications are the cornerstone of RA treatment and include:
NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): These provide pain relief and reduce inflammation but do not alter disease progression.
Corticosteroids: Used for short-term control of severe flare-ups, corticosteroids can rapidly diminish inflammation but are not suitable for long-term use due to side effects.
DMARDs (Disease-Modifying Anti-Rheumatic Drugs): These drugs, such as methotrexate, slow joint damage and disease progression. Regular monitoring is necessary due to potential side effects.
Biologic Agents: Target specific immune pathways to inhibit inflammation. Examples include infliximab, adalimumab, and etanercept. Biologics are often prescribed for patients who do not respond to traditional DMARDs.
Beyond medication, lifestyle adaptations can significantly improve symptoms and quality of life. These include:
Rest and activity balance: Adequate rest helps conserve energy, while gentle exercise maintains joint flexibility and muscle strength.
Physical therapy: Tailored exercises and stretching can improve joint function and reduce stiffness.
Supportive devices: Splints and braces can protect affected joints from undue stress.
Dietary measures: A nutritious diet rich in omega-3 fatty acids, proteins, and calcium can support joint health and overall well-being.
Stress management: Techniques like mindfulness, meditation, and stress reduction practices can help manage chronic pain and emotional health.
In some cases, joint damage may require surgical intervention, including joint replacement or repair, to restore function and relieve pain. Such procedures are typically considered after conservative treatments have failed and the disease has caused significant damage.
Regular checkups with your rheumatologist are essential for monitoring disease activity, adjusting treatments, and preventing complications. Educating yourself about RA and actively participating in your care enhances treatment outcomes.
In conclusion, while rheumatoid arthritis is a lifelong condition with no known cure, advances in medical treatments and supportive care can markedly improve patient outcomes. Early diagnosis, personalized treatment plans, lifestyle adaptations, and ongoing medical supervision are key to managing symptoms, preventing joint destruction, and maintaining a good quality of life.