Comprehensive Guide to Rheumatoid Arthritis: Causes, Symptoms, and Modern Treatment Options
This detailed guide explores rheumatoid arthritis, covering its causes, symptoms, and the latest treatment options. Understanding the disease helps patients manage symptoms effectively, prevent joint damage, and improve quality of life. From genetic factors to innovative therapies, learn everything about this chronic autoimmune condition in our comprehensive overview.
Comprehensive Guide to Rheumatoid Arthritis: Causes, Symptoms, and Modern Treatment Options
Rheumatoid arthritis (RA) is a complex and chronic autoimmune disorder that affects millions of individuals across the globe. Characterized by persistent inflammation primarily in the joints, RA can also involve various organs, including the eyes, lungs, cardiovascular system, and nerves. Unlike osteoarthritis, which results from wear and tear, rheumatoid arthritis involves an autoimmune response where the body's immune system mistakenly attacks its own tissues, leading to joint damage, deformities, and functional impairment. Understanding the root causes, common symptoms, and effective treatment strategies is essential for managing this condition effectively and improving patients' quality of life.
Unraveling the Causes of Rheumatoid Arthritis
The exact etiology of rheumatoid arthritis remains elusive; however, scientific research has identified several factors that appear to increase the risk of developing the disease. Genetics play a notable role, with specific gene markers such as the HLA-DRB1 gene being associated with increased susceptibility. Individuals with a family history of RA are at a higher risk, indicating a hereditary component.
Environmental influences are also significant contributors. Exposure to certain triggers like cigarette smoke, infections, and environmental pollutants may initiate or exacerbate the autoimmune process. Obesity has similarly been linked to higher disease activity, possibly due to increased systemic inflammation caused by excess adipose tissue. Additionally, hormonal factors and gender differences influence susceptibility, with women being disproportionately affected, suggesting a potential role of hormonal regulation in disease pathogenesis.
The immune system's dysregulation is central to RA development. In genetically predisposed individuals, environmental triggers may activate immune cells, leading to the production of autoantibodies such as rheumatoid factor (RF) and anti-cyclic citrullinated peptide (anti-CCP) antibodies. These autoantibodies target joint linings (synovium), culminating in inflammation and tissue destruction.
Recognizing the Symptoms of Rheumatoid Arthritis
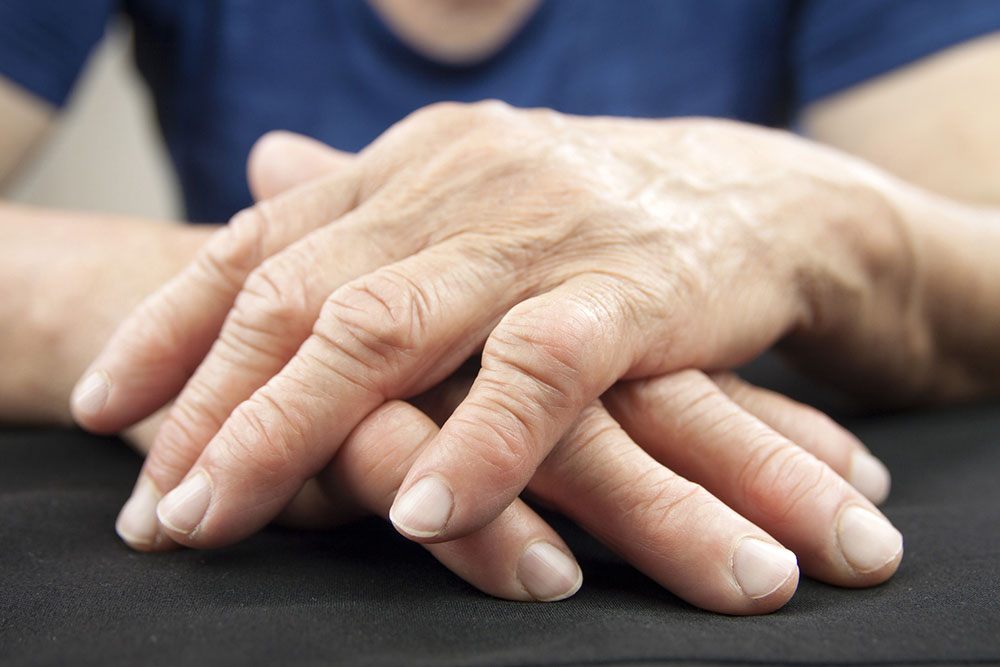
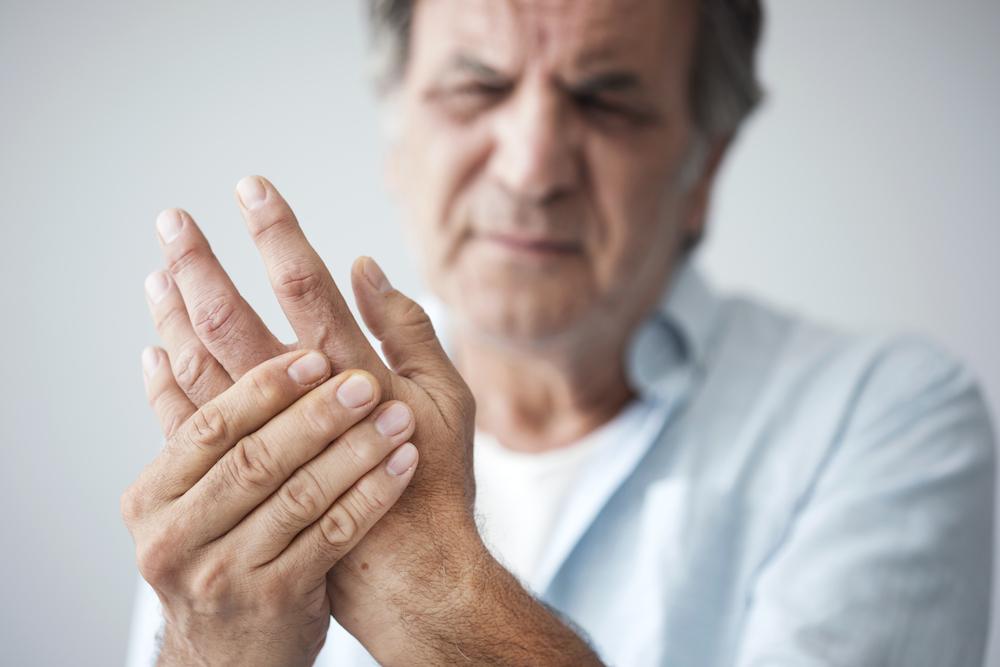
The clinical presentation of rheumatoid arthritis varies, but certain hallmark signs aid in diagnosis. Early symptoms typically include persistent joint swelling, localized pain, and stiffness, especially noticeable in the morning or after periods of inactivity. This stiffness often lasts more than an hour and gradually eases with movement. Patients may also experience systemic symptoms such as fatigue, low-grade fever, muscle aches, and general malaise.
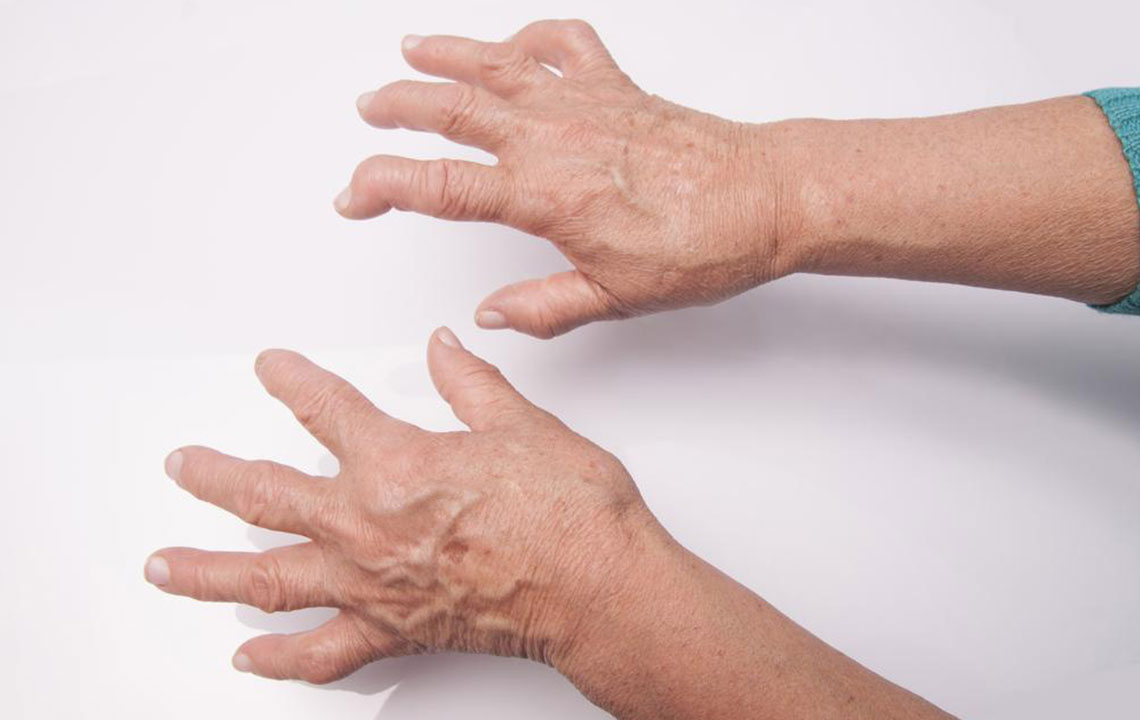
As the disease progresses, symmetrical joint involvement becomes apparent, affecting small joints like those in the fingers, wrists, and toes. Persistent inflammation can lead to joint deformation, subluxation, and loss of function. Beyond joints, RA may cause extra-articular manifestations, including skin nodules, eye dryness or inflammation, lung fibrosis, and cardiovascular issues. Recognizing these symptoms early is crucial for timely intervention and preventing irreversible joint damage.
Furthermore, laboratory tests, such as elevated inflammatory markers (ESR and CRP), and imaging studies like X-rays or ultrasound, support diagnosis and help assess disease severity. The presence of autoantibodies, notably RF and anti-CCP, strengthens the diagnosis of rheumatoid arthritis.
Modern Treatment Strategies for Managing Rheumatoid Arthritis
Managing rheumatoid arthritis requires a comprehensive approach tailored to disease severity, patient preferences, and comorbidities. The primary goal is to control inflammation, prevent joint damage, and maintain function. Treatment strategies encompass pharmacological options, lifestyle modifications, physical therapy, and, in some cases, surgical interventions.
Medications and Biological Therapies
Current pharmacotherapy involves disease-modifying antirheumatic drugs (DMARDs), which are foundational in RA management. Methotrexate remains the first-line DMARD, effectively reducing inflammation and slowing disease progression. Other conventional DMARDs include sulfasalazine and hydroxychloroquine. When monotherapy is insufficient, combination therapy with multiple DMARDs may be employed.
In recent years, biologic agents targeting specific immune pathways have revolutionized RA treatment. These include tumor necrosis factor (TNF) inhibitors such as infliximab, etanercept, and adalimumab, as well as interleukin inhibitors and Janus kinase (JAK) inhibitors. Biologics are particularly beneficial for patients with moderate to severe disease who do not respond to traditional DMARDs.
Physical Therapy and Lifestyle Adjustments
Alongside medications, physical and occupational therapy play vital roles in maintaining joint function and reducing stiffness. Regular exercise, tailored to individual capacity, can strengthen muscles, improve flexibility, and diminish fatigue. Weight management is also essential, as excess weight exacerbates joint strain and inflammation.
Additionally, adopting an anti-inflammatory diet rich in fruits, vegetables, omega-3 fatty acids, and whole grains can help modulate immune responses. Avoiding smoking and limiting alcohol intake are lifestyle modifications recommended to reduce disease severity and improve treatment outcomes.
Surgical Interventions
In cases where joint damage is severe or deformities threaten mobility, surgical options such as joint replacement or synovectomy may be considered. These procedures aim to restore function, relieve pain, and improve the patient’s overall quality of life.
Emerging Therapies and Research
Ongoing research continues to explore new treatment avenues, including regenerative medicine approaches, stem cell therapy, and personalized medicine based on genetic profiling. Advances in understanding the immunological mechanisms of RA promise to yield more targeted and less invasive treatments in the future.
Living with Rheumatoid Arthritis: Tips for Patients
Although rheumatoid arthritis is a lifelong condition, many patients lead active and fulfilling lives with proper disease management. Education about the disease, adherence to prescribed therapies, and regular medical follow-up are foundational to successful control.
Managing stress through relaxation techniques, engaging in suitable physical activities, and maintaining social connections contribute to overall well-being. Patients should work closely with their healthcare providers to tailor treatment plans and address any new symptoms promptly.
In conclusion, early diagnosis, comprehensive treatment, and lifestyle modifications are key to controlling rheumatoid arthritis and minimizing its impact on daily life. Continued research and advancements in medical therapies offer hope for improved outcomes and potentially curative interventions in the future.