Comprehensive Approaches to Managing Spondylolisthesis Symptoms for Improved Quality of Life
This comprehensive guide explores effective non-surgical and surgical strategies for managing spondylolisthesis. It highlights the importance of physical therapy, activity modifications, supportive devices, and surgical options to alleviate symptoms and improve quality of life. Emphasizing early diagnosis, lifestyle changes, and personalized treatment plans, the article aims to help patients better understand and manage this chronic spinal condition for enhanced mobility and overall well-being.
Effective Strategies for Managing Spondylolisthesis Symptoms
Spondylolisthesis is a chronic spinal condition characterized by one vertebra slipping forward over the vertebra beneath it. This condition can lead to lower back pain, muscle tightness, nerve compression, and significant mobility issues, affecting an individual's daily activities and overall quality of life. Understanding and managing this condition through various treatment approaches can significantly alleviate symptoms and promote better spinal health.
While some cases of spondylolisthesis require surgical intervention, many patients benefit from non-invasive treatments that focus on symptom management, pain relief, and strengthening the supporting muscles. This comprehensive guide explores effective non-surgical strategies, discusses when surgical options might be necessary, and offers practical tips for maintaining spinal health.
Understanding Spondylolisthesis
Spondylolisthesis occurs when a vertebra slips out of its normal position, typically in the lumbar spine (lower back). The severity ranges from mild slips that cause minimal discomfort to severe cases that can impair mobility dramatically. Causes include congenital defects, stress fractures from repetitive activity, degenerative changes in aging, or traumatic injuries.
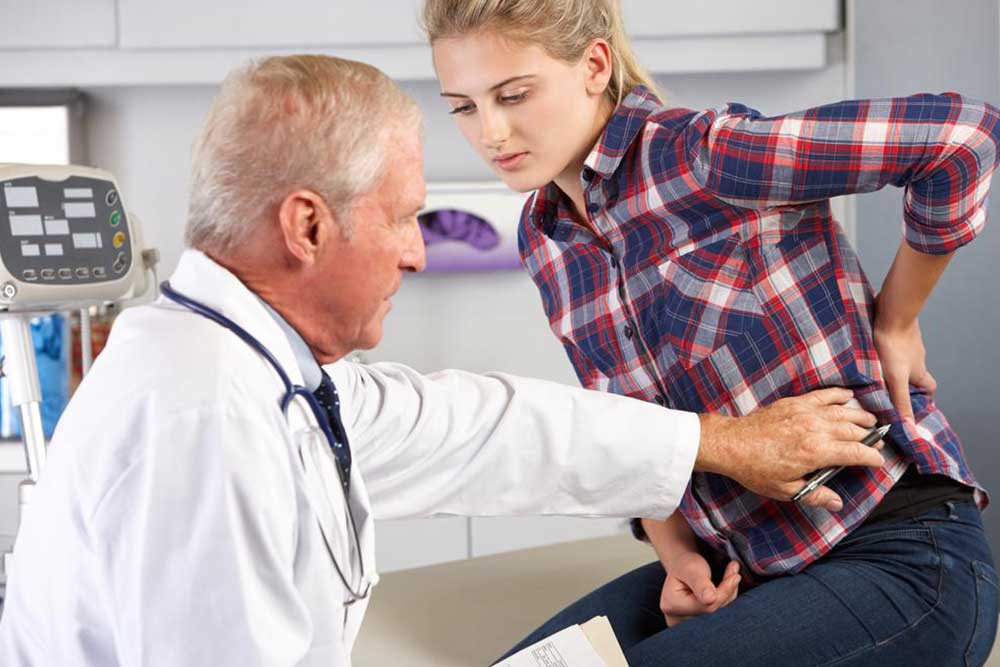
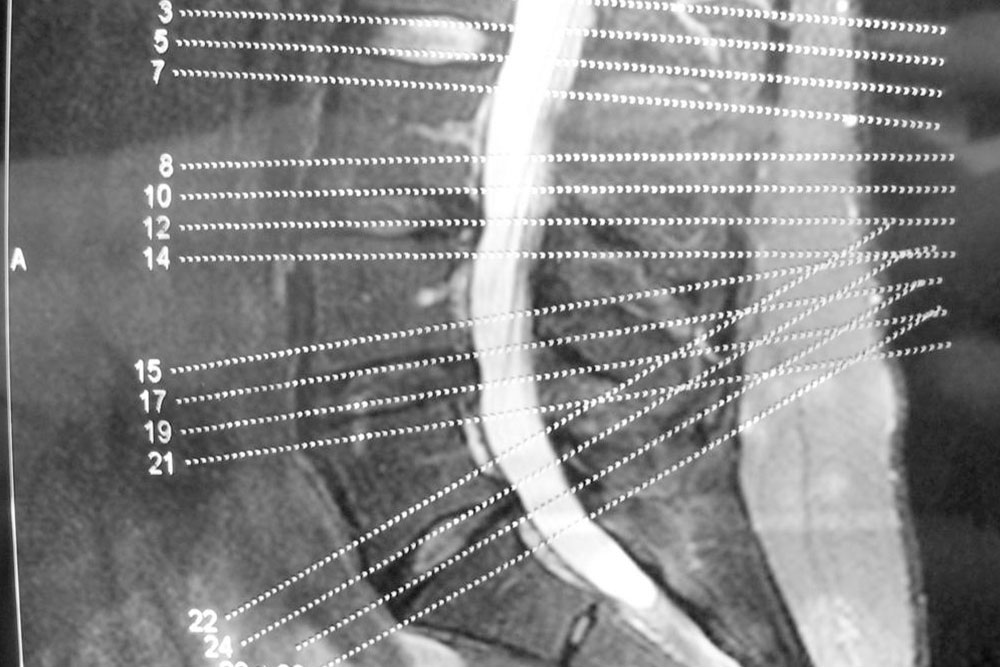
Symptoms often include persistent lower back pain, a feeling of instability or weakness in the legs, numbness, tingling sensations, and difficulty standing or walking for prolonged periods. Diagnosing the condition typically involves physical evaluation and imaging studies such as X-rays, MRI, or CT scans to assess the extent of vertebral displacement and nerve involvement.
Non-Surgical Management of Spondylolisthesis
Many individuals with spondylolisthesis can effectively manage their symptoms without resorting to surgery. Conservative treatment plans focus on easing pain, reducing inflammation, and strengthening the muscles that support the spine. These approaches aim to enhance mobility, prevent further vertebral slipping, and improve overall life quality.
1. Physical Therapy and Exercise Programs
Physical therapy plays a pivotal role in managing spondylolisthesis. Certified physical therapists design individualized exercise regimens tailored to the patient's specific needs. The primary goal is to strengthen core muscles—especially the abdominals and lower back—to support spinal stability. Additionally, stretching tight hamstrings and hip flexors can reduce stress on the lower back, alleviating pain and stiffness.
Typical physical therapy programs last between 6 to 12 weeks and include exercises such as pelvic tilts, bridges, knee-to-chest stretches, and gentle back extensions. These exercises improve flexibility, muscular balance, and posture, which collectively decrease spinal load and diminish discomfort. Regular sessions combined with home exercises can help maintain progress and prevent symptom exacerbation.
2. Activity Modification and Support Devices
Adapting daily activities is crucial in avoiding movements that aggravate symptoms. Patients are encouraged to avoid heavy lifting, twisting motions, and high-impact activities that strain the lower back. Incorporating low-impact exercises like swimming, water aerobics, or Tai Chi can promote spinal health without undue stress.
Support braces or lumbar belts are often recommended to provide additional stability during activity. These devices can help prevent abnormal spinal motion and reduce pain, especially during prolonged standing or physical exertion. The duration for wearing braces varies based on individual needs and treatment plans.
3. Heat and Cold Therapy
Applying heat packs can relax tense muscles, increase blood flow, and promote healing. Cold packs help reduce inflammation, swelling, and numb localized pain. Alternating between heat and cold therapies can provide comprehensive relief from discomfort, especially during flare-ups. Patients should follow recommendations for duration and frequency to avoid skin irritation or other adverse effects.
Surgical Options for Severe or Refractory Cases
When conservative treatments do not provide sufficient relief, or when the severity of vertebral slippage causes significant nerve compression or instability, surgery may be indicated. Surgical interventions aim to stabilize the spine, relieve nerve pressure, and prevent further vertebral slipping.
1. Spinal Fusion Surgery
Spinal fusion involves joining two or more vertebrae to eliminate movement between them, thereby stabilizing the spinal segment. This procedure is often performed in high-grade spondylolisthesis and can significantly reduce pain by preventing further slippage. However, it also reduces overall spinal flexibility, which must be considered when planning treatment.
2. Spinal Decompression Procedures
In cases where nerve compression causes severe pain, numbness, or weakness, decompression surgery may be necessary. This involves removing parts of the affected vertebrae, disks, or bone spurs to alleviate pressure on nerve roots. Techniques include laminectomy or discectomy, depending on the structural issues involved.
Recovery from surgery involves a period of rest, followed by gradual physical activity. Postoperative exercises are designed to restore strength and flexibility while avoiding strain on the healing spine. Patients are typically advised to engage in gentle stretching routines, such as knee-to-chest stretches, leg lifts, glute and hamstring stretches, and pelvic tilts, under professional guidance.
Maintaining a Healthy Spine
Long-term management of spondylolisthesis also includes lifestyle modifications. Maintaining a healthy weight reduces unnecessary stress on the lower back. Proper ergonomics during daily activities, such as correct posture while sitting, standing, and lifting, can significantly prevent symptom worsening.
Regular exercise, a balanced diet rich in anti-inflammatory nutrients, and staying well-hydrated support spinal health. Patients should consult healthcare professionals to develop a comprehensive management plan tailored to their specific condition and lifestyle.
Conclusion
Managing spondylolisthesis effectively requires a combination of approaches tailored to the severity of the condition and individual patient needs. Non-invasive therapies such as physical therapy, activity modification, and supportive devices often suffice to control symptoms and improve mobility. When these options are insufficient, surgical interventions can provide lasting relief and spinal stability. Early diagnosis and consistent management are key to maintaining quality of life and preventing further complications associated with this chronic spinal condition.