Comprehensive Guide to Fungal Nail Infections: Causes, Prevention Strategies, and Effective Treatments
This comprehensive guide provides detailed insights into fungal nail infections, detailing their causes, risk factors, prevention strategies, and an overview of effective treatments. Whether mild or severe, understanding these aspects helps in timely management and reduces recurrence risk, particularly for vulnerable populations. Explore modern and traditional treatment options, along with practical prevention tips, to maintain healthy, fungus-free nails and avoid complications.

Understanding Fungal Nail Infections: Causes, Prevention, and Treatment Options
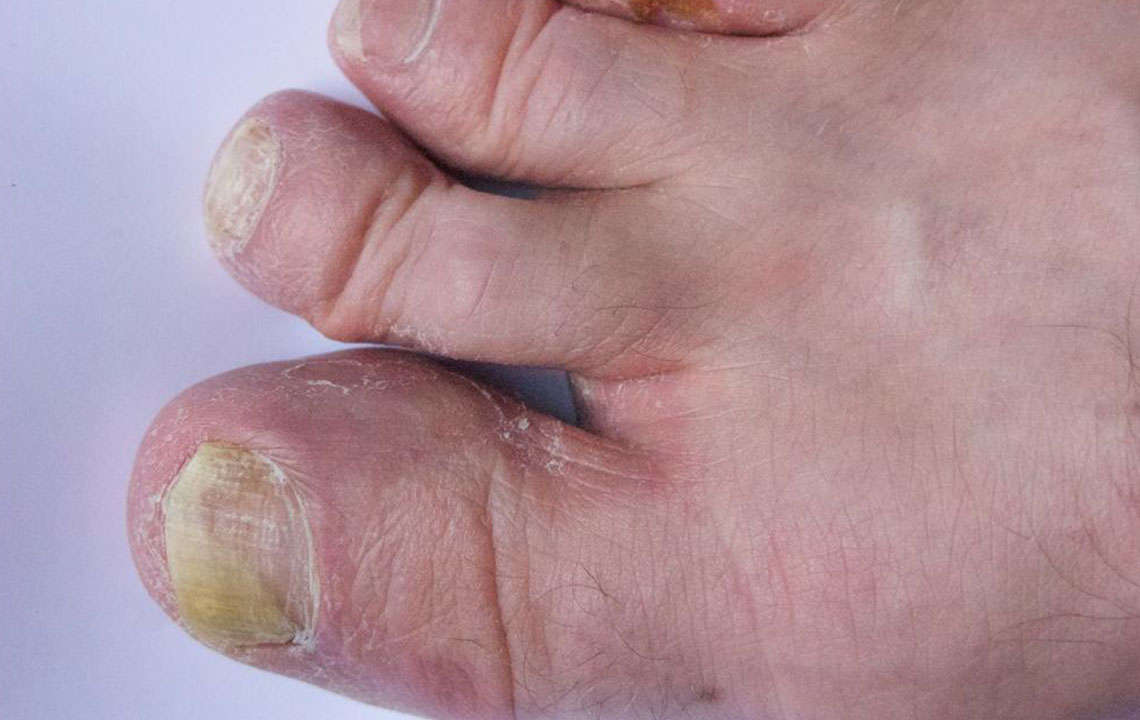
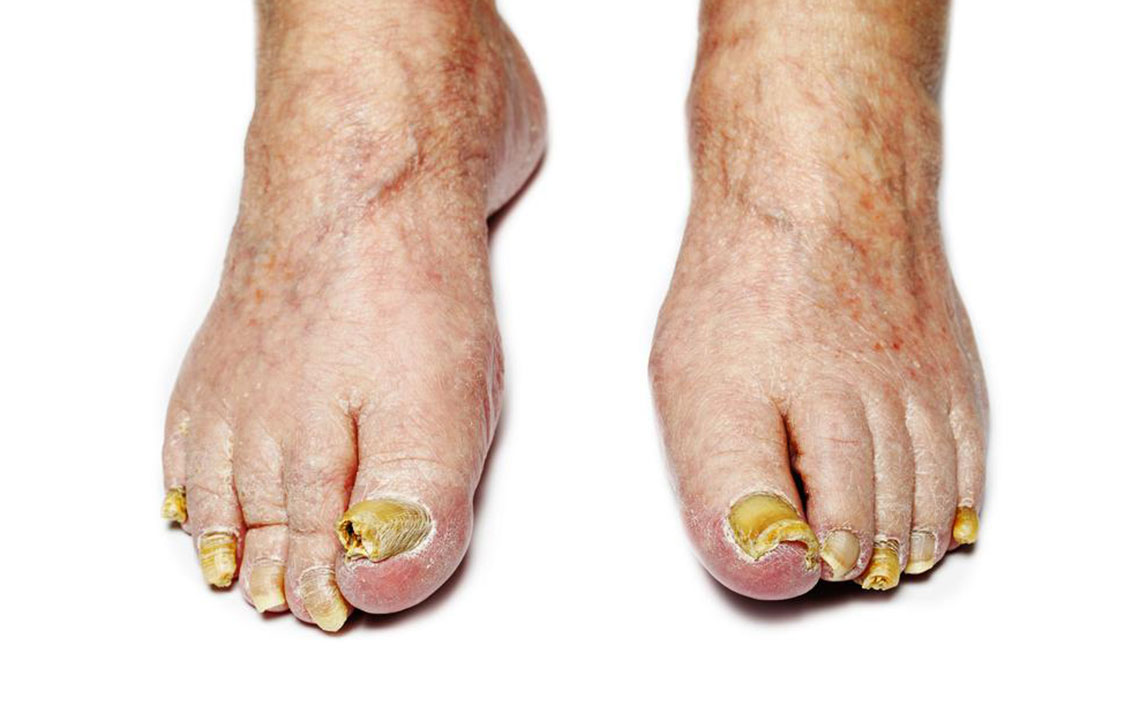
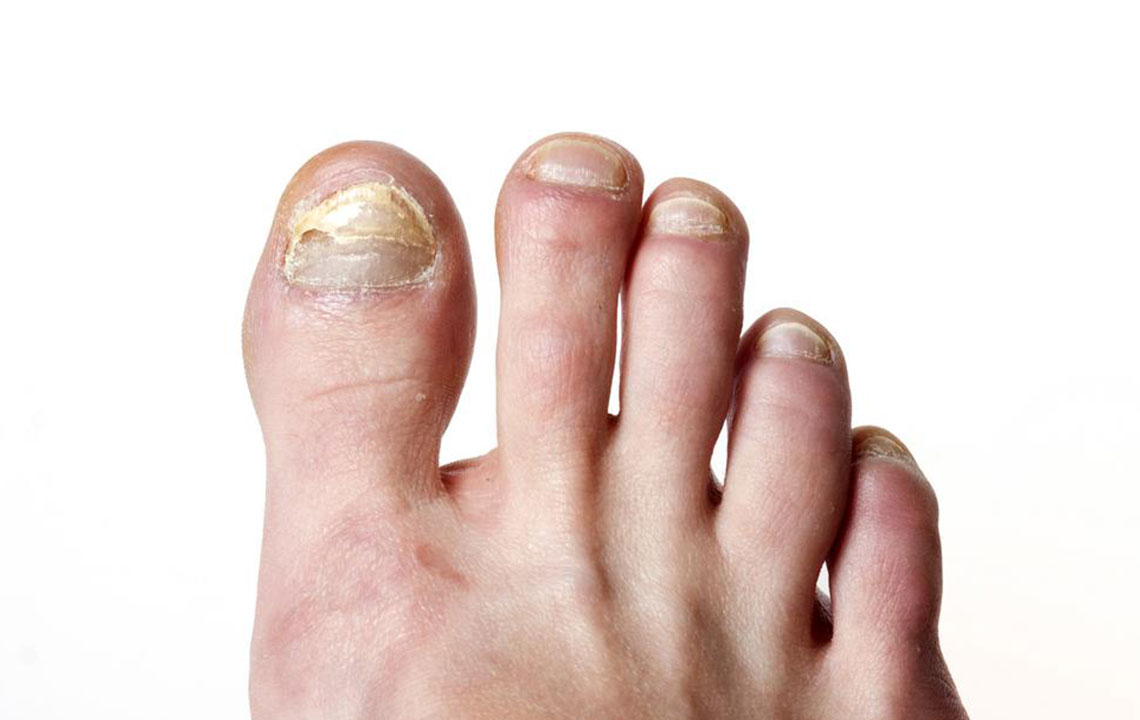
Nail fungal infections, medically known as onychomycosis, are common conditions that occur when fungi infect the nails of the toes or fingers. These infections develop gradually and are often characterized by thickened, discolored, and brittle nails. The fungi responsible for these infections thrive in warm, moist environments, making our feet particularly vulnerable, especially in certain circumstances. Recognizing the causes, risk factors, prevention methods, and available treatments is essential for effective management and to prevent complications. In this comprehensive article, we delve into the details of fungal nail infections to help you understand how to protect your nails and seek appropriate treatment when necessary.
What are the primary causes of toenail fungal infections?
Toenail fungal infections are predominantly caused by various fungi, including dermatophytes, yeasts, and molds. Among these, dermatophytes are the most common culprits, typically originating from athlete’s foot infections and spreading to toenails over time. The fungi invade the nail bed, nail plate, or surrounding tissues, resulting in visible symptoms such as discoloration, thickening, and crumbling nails. While many factors contribute to fungal growth, some individuals are more susceptible due to genetic or environmental reasons.
Men tend to be affected more frequently than women by these infections, and adult populations are particularly at risk. The initiation and recurrence of toenail fungal infections are often linked to underlying health conditions, such as diabetes and circulatory disorders, which compromise the immune system and reduce the body’s ability to fight off fungal invasions. Additionally, environmental factors play a significant role. For example, walking barefoot in communal showers, gyms, or swimming pools exposes individuals to fungi and increases the likelihood of infection. Wearing ill-fitting shoes that cause sweating and create moist environments around the toenails further facilitates fungal proliferation.
The primary fungi involved include:
Dermatophytes: The leading cause, often associated with athlete’s foot and other skin fungal infections.
Yeasts: Less common but capable of infecting nails, especially in immunocompromised individuals.
Molds: Contribute to more severe or atypical fungal infections, often seen in chronic cases.
Understanding these causative agents helps in tailoring appropriate treatment strategies, as different fungi respond variably to therapies. Preventing fungal infections involves both reducing exposure to fungi and maintaining good foot hygiene.
Who is most susceptible to toenail fungal infections?
While anyone can develop a fungal nail infection, certain groups are at a higher risk. These include:
Older Adults: Aging causes slower nail growth, brittle nails, and poorer circulation, making it easier for fungi to invade.
People with Pre-existing Conditions: Individuals with diabetes, peripheral vascular disease, or immune suppression are more vulnerable due to compromised immune defenses.
Individuals Wearing Artificial Nails or Constrictive Footwear: These can trap moisture and prevent proper foot hygiene, promoting fungal growth.
Persons with Nail or Skin Injuries: Breaks in the skin or nails provide an entry point for fungi.
Family Members with a History of Fungal Infections: Fungal spores can easily spread within households or communal environments.
Preventive measures should be especially emphasized for these at-risk populations to minimize infection incidence.
Effective Management of Toenail Fungal Infections
Addressing toenail fungus involves a combination of medical treatment, lifestyle modifications, and preventive practices. The challenge lies in the fact that fungal infections tend to recur if not properly treated, and some cases can lead to permanent nail damage. Early detection and intervention are key to effective management.
Medical Treatment Options
Conventional treatment approaches include oral antifungal medications such as terbinafine, itraconazole, or fluconazole, which are often prescribed for persistent or severe infections. Compared to over-the-counter remedies, these medications tend to be more effective but may require monitoring due to potential side effects. Topical antifungal solutions and nail lacquers, like ciclopirox or amorolfine, can be used for mild to moderate cases, typically applied over a period of several months. Sometimes, combination therapy yields the best results.
Lifestyle and Home Care Strategies
Keeping nails healthy and reducing the risk of fungal growth involves regular trimming, proper foot hygiene, and moisture control. Ensure your feet are thoroughly dried after bathing or sweating, especially between the toes. Switching from closed-toe shoes to breathable footwear and using moisture-wicking socks also minimizes fungal-friendly environments. Avoid sharing nail clippers, towels, or shoes to prevent cross-infection. Applying antifungal powders or sprays within footwear can help control fungal spores.
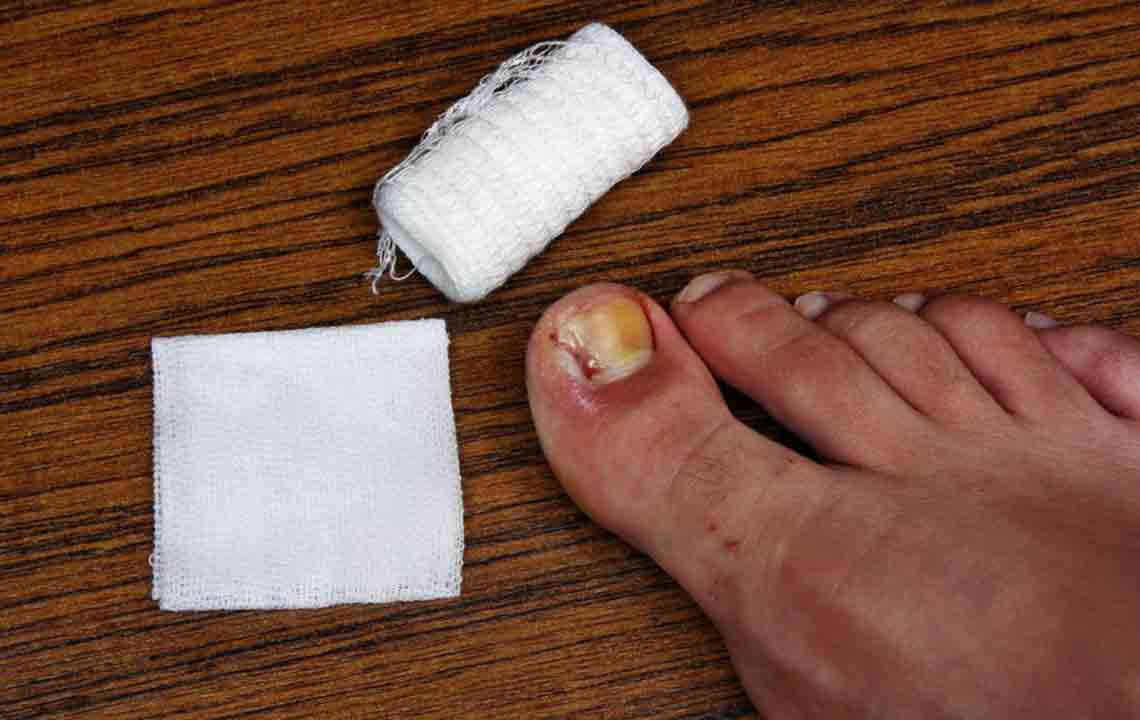
Invasive Treatments
In stubborn cases, surgical removal of the affected nail may be necessary to eliminate the infection completely. This procedure is often combined with systemic antifungal therapy to prevent recurrence. Nail removal can provide a temporary solution while the new, healthy nail regrows, but it requires proper aftercare and monitoring.
Home Remedies and Alternative Treatments
Various natural remedies such as vinegar soaks, tea tree oil, coconut oil, and cedar leaf oil are popular among many patients. While anecdotal evidence suggests some benefits, scientific validation remains limited. These remedies may help soften thickened nails or provide antifungal properties but should not replace medical treatments, especially in severe cases. Always consult your healthcare provider before trying home remedies to avoid potential irritation or contraindications.
Preventive Measures to Protect Your Nails
Prevention remains the best strategy against fungal nail infections. Wearing protective gloves when working with water or chemicals, regularly disinfecting footwear, opting for moisture-wicking socks, and avoiding walking barefoot in public spaces are simple yet effective steps. Choosing reputable salons that follow sterilization protocols can prevent iatrogenic fungal infections. Limiting the use of artificial nails and maintaining overall foot hygiene are also critical measures.
Emerging and Advanced Treatment Methods
Advances in technology have introduced new options for managing toenail fungi:
Laser and Light-Based Therapies: These treatments utilize focused laser energy or other light sources to eradicate fungi within the nail bed. They are non-invasive, relatively quick, and often require no anesthesia, making them attractive options for many patients.
Iontophoresis: This technique uses electrical currents to enhance the absorption of antifungal medications directly into the infected tissues, increasing treatment efficacy.
Nail Lacquers and Topical Agents with Novel Formulations: Emerging formulations aim to create inhospitable environments for fungi within the nail matrix, improving penetration and durability.
Prompt treatment and adopting preventive habits are essential to controlling toenail fungal infections and avoiding complications, particularly in individuals with underlying health conditions like diabetes. Consulting a healthcare professional for an accurate diagnosis and personalized treatment plan is highly recommended.