Comprehensive Guide to Crohn's Disease: Symptoms, Types, and Effective Management Strategies
Crohn's disease is a long-term inflammatory condition affecting the digestive tract, leading to symptoms like abdominal pain, diarrhea, and weight loss. This comprehensive guide details the disease's symptoms, types, risk factors, and management strategies, emphasizing personalized treatment and lifestyle adjustments. While incurable, modern therapies including medications, biologics, and surgery help control symptoms and improve quality of life. Awareness of risk factors such as genetics and environmental influences is vital for early detection. With proper care, many patients maintain active lives despite the chronic nature of Crohn's disease.

Comprehensive Guide to Crohn's Disease: Symptoms, Types, and Effective Management Strategies
Crohn's disease, also known as regional enteritis or ileitis, is a chronic inflammatory condition that primarily affects the gastrointestinal (GI) tract. As a subtype of inflammatory bowel disease (IBD), Crohn's causes persistent inflammation and swelling along the digestive system, leading to a range of uncomfortable and sometimes debilitating symptoms. Although the exact cause remains unknown, current research indicates that genetics, immune system dysfunction, environmental factors, and lifestyle choices all play a role in its development. This comprehensive guide aims to shed light on the symptoms, different types, risk factors, and available treatment options to better equip patients and caregivers in managing this complex disease effectively.
Recognizing the Symptoms of Crohn's Disease
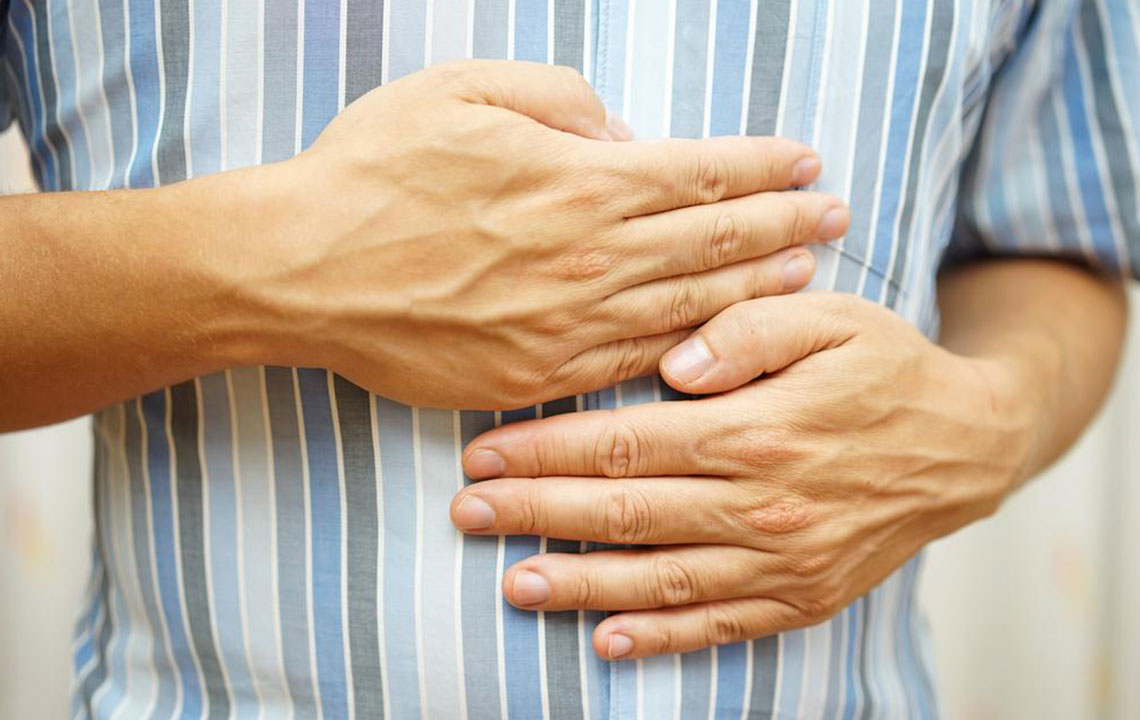
Understanding the symptoms of Crohn's disease is crucial for early diagnosis and effective treatment. The presentation of symptoms can vary significantly from person to person, often developing gradually but sometimes appearing abruptly. Early signs frequently include persistent diarrhea, which may be accompanied by abdominal pain or cramps. Patients often experience rectal bleeding, which is a red flag indicating inflammation or ulceration within the GI tract. Other common initial symptoms include fever, fatigue, loss of appetite, unintentional weight loss, and a sensation of bowel fullness or urgency. These symptoms can impair daily activities and overall well-being.
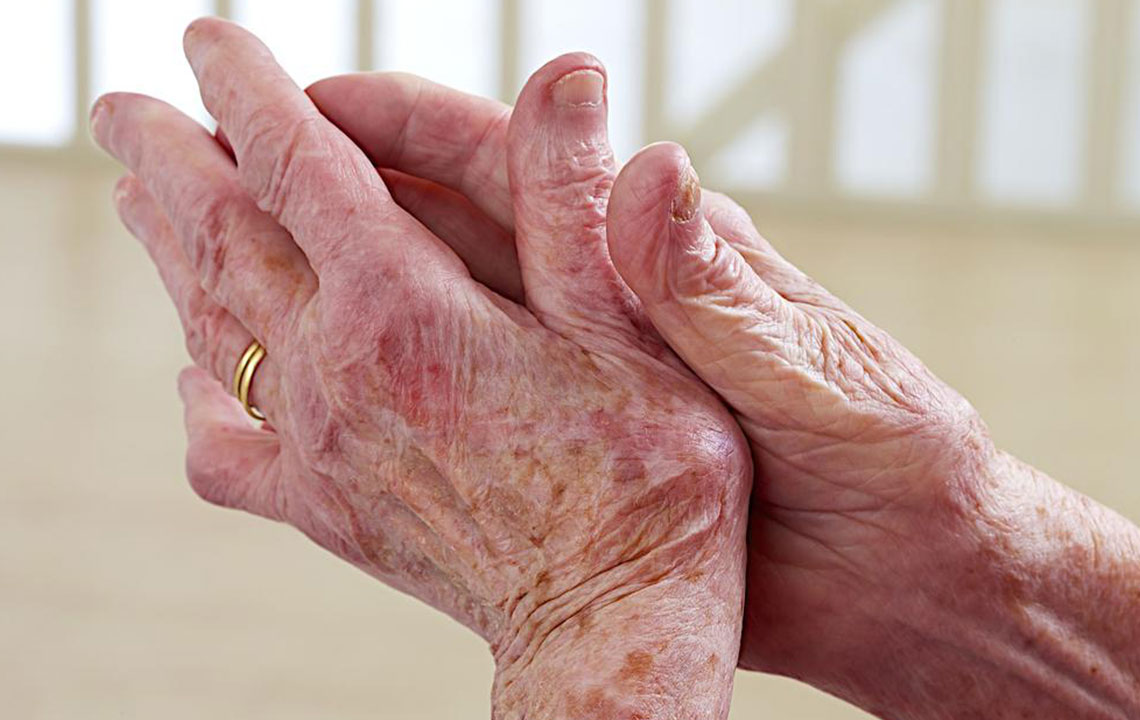
As the disease progresses or in more severe cases, additional symptoms may manifest, including the formation of anal fistulas—abnormal connections between the intestine and other organs or skin—ulcers on various parts of the body from mouth to anus, skin rashes, joint inflammation, and anemia. Anemia, which results from chronic blood loss or malabsorption of nutrients, can cause symptoms such as breathlessness, dizziness, and reduced physical endurance. The early recognition of these symptoms and prompt consultation with healthcare professionals are essential for timely diagnosis and intervention, potentially reducing the risk of complications and improving quality of life.
Different Types of Crohn's Disease
Crohn's disease can affect various regions within the gastrointestinal system, leading to classification into several distinct types based on the location and pattern of inflammation. Understanding these types helps in tailoring treatment strategies and predicting disease course. The main categories include:
Ileocolitis: This is the most common form, involving inflammation of the ileum—the final section of the small intestine—and the beginning part of the colon. Symptoms often include right lower abdominal pain, diarrhea, and weight loss.
Ileitis: Characterized solely by inflammation of the ileum, this type can cause persistent right-sided abdominal pain and diarrhea, often with less involvement of the colon.
Gastroduodenal Crohn’s Disease: Affecting the stomach and the upper part of the small intestine (duodenum), this form leads to upper abdominal discomfort, nausea, vomiting, and sometimes nutritional deficiencies due to impaired digestion.
Jejunoileitis: This type features patchy inflammation within the jejunum, a mid-section of the small intestine, and can result in diarrhea, malabsorption, and nutritional deficiencies.
These classifications assist healthcare providers in determining the most effective treatment plans and predicting possible complications based on disease localization.Management and Treatment Options for Crohn's Disease
While there is currently no cure for Crohn's disease, advances in medical science have provided a variety of treatment options aimed at controlling inflammation, relieving symptoms, and preventing complications. The primary goal of treatment is to induce remission—where symptoms are minimized or absent—and to maintain this state over the long term to enhance the patient's quality of life. A multidisciplinary approach involving medication, lifestyle adjustments, and sometimes surgical intervention is often necessary.
Medical treatments include:
Anti-inflammatory Drugs: These are usually the first line of therapy and include aminosalicylates such as mesalamine, which help reduce inflammation in the intestinal lining.
Immunosuppressants: Agents like azathioprine, mercaptopurine, or methotrexate suppress overactive immune responses that lead to inflammation. These medications require close monitoring due to potential side effects like liver toxicity or increased infection risk.
Biologic Therapies: These are advanced drugs, such as infliximab and adalimumab, designed to target specific proteins involved in the inflammatory process (like TNF-alpha). Biologics can be highly effective in inducing and maintaining remission, especially in severe cases.
Antibiotics: Used primarily to manage complications such as abscesses or fistulas, antibiotics help reduce bacterial activity and control secondary infections.
Surgical Intervention: Surgery may be necessary when medications fail or complications like strictures, fistulas, or perforations occur. Procedures include removing damaged sections of the intestine, draining abscesses, or repairing fistulas. Notably, surgery does not cure Crohn's disease but can significantly improve quality of life. Approximately 50% of patients might require surgical management during their illness.
Additionally, lifestyle modifications are crucial. Dietary adjustments, smoking cessation, stress management, and regular monitoring help in managing flares and maintaining remission. Personalized treatment plans are essential, as the disease varies greatly among individuals.Factors Contributing to Crohn's Disease Risk
Understanding what increases the likelihood of developing Crohn's disease can help in preventive efforts. Several factors have been identified as increasing the risk, including:
Genetics: Family history plays a significant role, with individuals having a higher chance of developing Crohn's if relatives are affected. Specific gene mutations such as NOD2/CARD15 are associated with increased susceptibility.
Environmental Factors: Smoking is a well-documented risk factor, with smokers more prone to severe disease and complications. Urban living and Westernized dietary habits—particularly diets high in processed and fatty foods—also contribute to risk.
Medications: Use of certain drugs like antibiotics, oral contraceptives, aspirin, and NSAIDs (non-steroidal anti-inflammatory drugs) may slightly elevate the risk by influencing gut flora and immune responses.
Dietary Factors: Diets rich in fats and low in fiber have been linked to a higher incidence of Crohn's disease, possibly due to alterations in gut microbiota and immune activation.
Living with Crohn's disease can be challenging, with potential flare-ups and frequent medical checkups. However, with ongoing medical advancements and proper management—including medication adherence, lifestyle modifications, and regular monitoring—patients can lead active and fulfilling lives despite the chronic nature of the condition.