Comprehensive Guide to Psoriatic Arthritis: Recognizing Symptoms and Managing the Disease
This comprehensive article provides insights into psoriatic arthritis, including key symptoms, potential complications, and management strategies. Understanding the signs such as joint pain, dactylitis, and enthesitis can help in early diagnosis and effective treatment. The article emphasizes the importance of medical checkups to prevent serious complications like eye inflammation and cardiovascular issues associated with psoriatic arthritis. Whether you have psoriasis or joint symptoms, recognizing these signs early can significantly improve your quality of life and joint health.

Comprehensive Guide to Psoriatic Arthritis: Recognizing Symptoms and Managing the Disease
Psoriatic arthritis (PsA) is a chronic inflammatory condition that primarily affects the joints and is often associated with psoriasis, a skin disorder characterized by red, scaly patches. This autoimmune disease involves joint pain, swelling, and stiffness resulting from inflammation, which can significantly diminish quality of life if not diagnosed and managed appropriately. While psoriasis appears on areas such as elbows, knees, scalp, or back, some individuals develop psoriatic arthritis without skin manifestations or may experience joint symptoms prior to the skin changes becoming evident.
Recognizing the Signs and Symptoms of Psoriatic Arthritis
Psoriatic arthritis can affect individuals across all age groups and genders. Although it is commonly linked with psoriasis, it's important to understand that some affected individuals may develop other forms of arthritis, such as rheumatoid arthritis or osteoarthritis, independently of psoriasis. Recognizing the early symptoms of psoriatic arthritis is crucial for timely treatment and preventing joint damage.
Key symptoms associated with psoriatic arthritis include:
Persistent joint pain and swelling, often accompanied by stiffness, especially in the morning or after periods of inactivity.
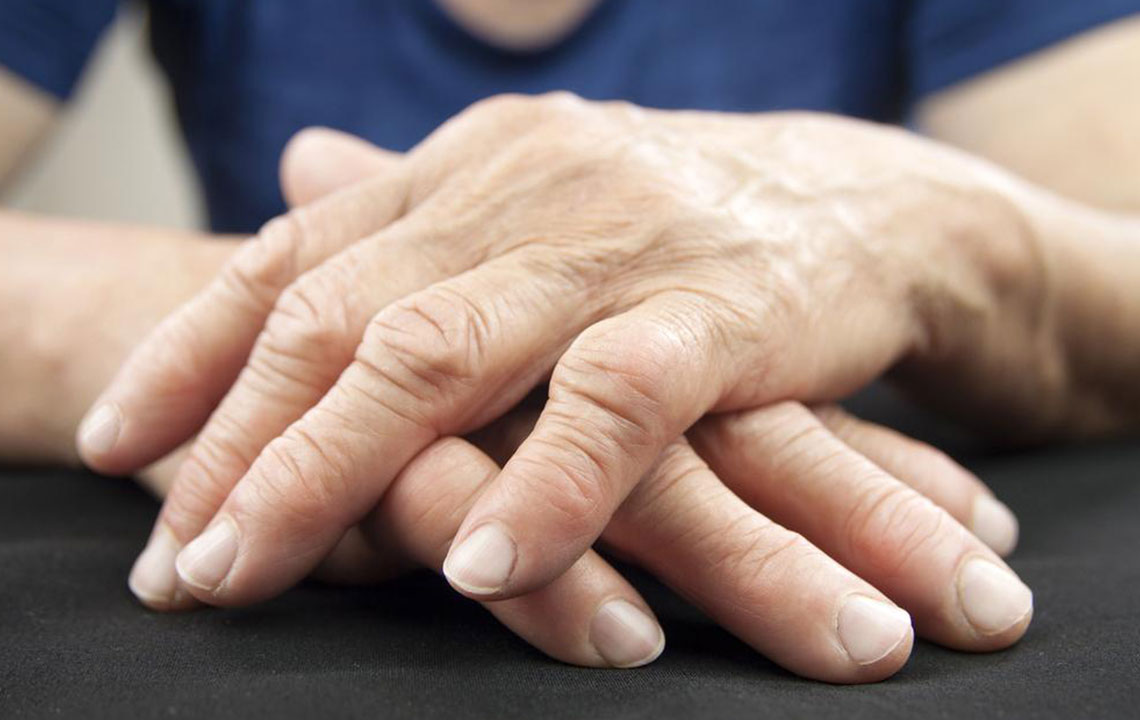
Swelling of fingers and toes, medically termed dactylitis, caused by inflammation of the entire digit.
Lower back, buttocks, and neck pain resulting from spinal inflammation, a condition known as spondylitis, which can lead to stiffness and reduced mobility.
Pain and swelling at the Achilles tendons’ attachment points at the heels, leading to heel pain and difficulty walking.
Enthesitis, which is inflammation at the sites where tendons or ligaments connect to bones, contributing to pain in various locations.
These symptoms frequently involve other parts such as the chest, knees, and hips. Beyond joint discomfort, psoriatic arthritis can cause nail abnormalities, including thickening and pitting, along with general fatigue that worsens over time, often exacerbated by emotional stress and disease progression.It's important to note that psoriatic arthritis can affect up to 78 different joint sites throughout the body. While some joints are more susceptible, particularly the distal interphalangeal joints of the fingers and toes, others like the knees, hips, and spine can also be involved. Approximately 25% of patients report experiencing neck or back pain, highlighting the disease’s potential to impact multiple skeletal regions.
Additional Effects and Complications of Psoriatic Arthritis
Although psoriatic arthritis typically spares major organs, it can sometimes lead to extra-articular complications. One notable issue is ocular inflammation, such as uveitis or iritis, which affects the eye’s uveal tract and can threaten vision if left untreated. Prompt diagnosis and treatment are vital to prevent permanent eye damage. Additionally, psoriatic arthritis increases the risk of cardiovascular diseases, including coronary artery disease and stroke, emphasizing the importance of regular health monitoring. Patients are advised to undergo routine medical checkups to identify any emerging complications early and to manage them effectively.
Managing psoriatic arthritis involves a multifaceted approach, including medication, lifestyle modifications, and regular medical supervision. Disease-modifying antirheumatic drugs (DMARDs), biologic agents, physical therapy, and lifestyle changes such as diet and exercise can significantly improve symptoms and prevent joint damage. Awareness of the disease's signs and symptoms facilitates early diagnosis, which can make a substantial difference in long-term outcomes. If you notice persistent joint pain, swelling, or skin changes, consulting a healthcare professional promptly is essential for appropriate evaluation and treatment planning.