In-Depth Guide to Managing Lupus and Rheumatoid Arthritis Treatments
Explore comprehensive strategies for managing lupus and rheumatoid arthritis, including medication options, latest therapies, lifestyle tips, and monitoring techniques to improve patient outcomes and quality of life.
Comprehensive Approaches to Treating Lupus and Rheumatoid Arthritis
Autoimmune diseases such as Systemic Lupus Erythematosus (SLE) and Rheumatoid Arthritis (RA) require tailored treatment strategies aimed at controlling symptoms, minimizing flare-ups, and slowing disease progression. While there is currently no definitive cure for lupus, advances in medical therapies have significantly improved the quality of life for patients. Managing these chronic conditions involves a combination of medications, lifestyle adjustments, and ongoing monitoring by healthcare professionals.
Lupus is characterized by the immune system attacking healthy tissues, leading to widespread inflammation and organ damage. Treatment plans must be highly individualized, depending on the severity of symptoms, the organs involved, and the frequency of flare-ups. Common medications used to manage lupus include Nonsteroidal Anti-Inflammatory Drugs (NSAIDs), antimalarials, corticosteroids, and immunosuppressants. Each of these drugs serves a specific purpose, with their benefits carefully weighed against potential side effects.
NSAIDs, such as ibuprofen and naproxen, are often the first line of defense for symptom relief. They help reduce inflammation, relieve pain, and lower fever. However, prolonged use of NSAIDs can pose risks such as gastrointestinal bleeding, kidney impairment, and cardiovascular issues. To mitigate these risks, healthcare providers may recommend the lowest effective doses and regular monitoring.
Antimalarial medications like hydroxychloroquine have been proven effective in reducing symptoms, preventing flares, and improving long-term outcomes in lupus patients. These drugs are generally well-tolerated but can cause side effects including stomach upset, skin rashes, and in rare cases, retinal toxicity. Regular eye examinations are recommended for patients on long-term hydroxychloroquine therapy to detect any early signs of eye damage.
Given the immune system's overactivity in lupus, immunosuppressants form an essential part of many treatment regimens. Drugs such as azathioprine, mycophenolate mofetil, and methotrexate are frequently prescribed to suppress immune responses and prevent organ damage. These medications, while effective, come with substantial risks like increased susceptibility to infections, liver toxicity, bone marrow suppression, and even a higher risk of certain cancers. Therefore, close monitoring is crucial during therapy.
In recent years, targeted biological therapies have emerged as promising options for managing severe or resistant lupus. Belimumab, a monoclonal antibody that inhibits B-lymphocyte stimulator (BLyS), has been approved for active lupus patients who are not responding well to standard treatments. Other agents, such as Rituximab, are currently under investigation and show potential for future use, aiming to provide more precise immune modulation with fewer side effects.
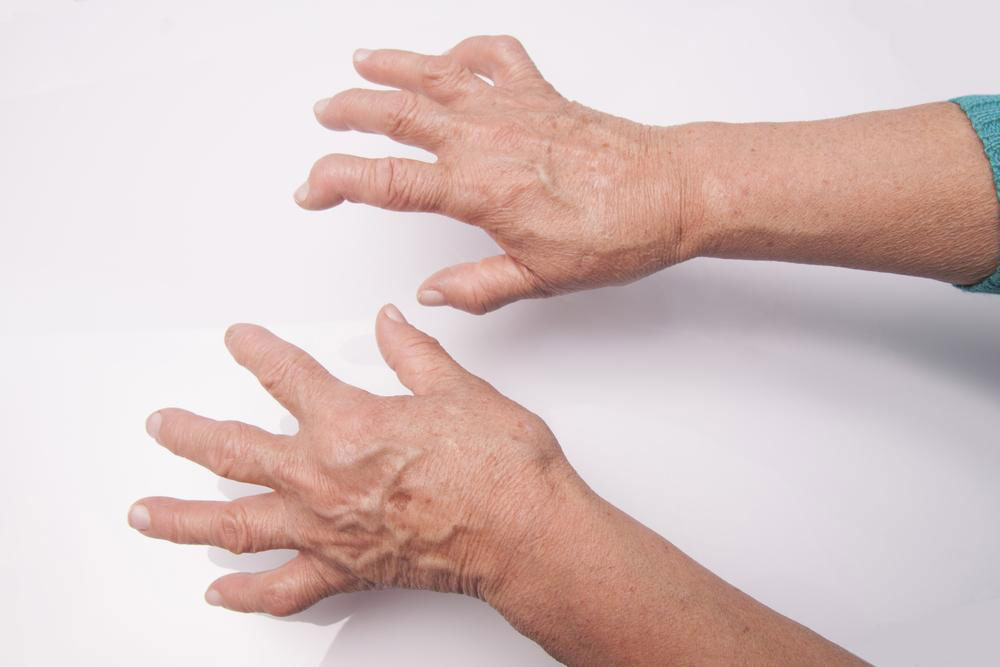
Turning to Rheumatoid Arthritis, the goal of treatment is to alleviate pain, reduce swelling, and prevent joint destruction. NSAIDs and corticosteroids often provide initial relief, but their long-term use carries notable side effects, including osteoporosis, weight gain, and increased infection risk. To achieve better disease control, Disease-Modifying Antirheumatic Drugs (DMARDs) are the mainstay of therapy. Methotrexate remains the most widely used DMARD, effectively slowing disease progression and preserving joint function. Other medications include leflunomide, sulfasalazine, and hydroxychloroquine, each with distinct mechanisms and side effect profiles.
Biologic agents have revolutionized RA management by targeting specific immune pathways involved in joint inflammation. Drugs like abatacept, adalimumab, infliximab, and tocilizumab focus on cytokines and immune cells that drive the disease process. These biologics can significantly reduce joint damage and improve quality of life but are associated with increased risks of infections and other immune-related complications. Combining biologics with traditional DMARDs, especially methotrexate, enhances their efficacy and safety profile.
Overall, effective management of lupus and RA requires a comprehensive understanding of the disease mechanisms, potential treatment options, and vigilant monitoring for side effects. Patients should work closely with their healthcare team to tailor treatment plans that balance efficacy and safety, aiming for remission or low disease activity and improved daily functioning. Lifestyle modifications, including diet, exercise, stress management, and avoiding triggers, are also critical components of a holistic approach to managing these chronic autoimmune conditions.
Advances in medical research continue to provide hope for better, more targeted therapies in the future. Patients are encouraged to stay informed about emerging treatments and participate in clinical trials when appropriate, as this can contribute to the development of more effective and safer therapies for lupus and rheumatoid arthritis.