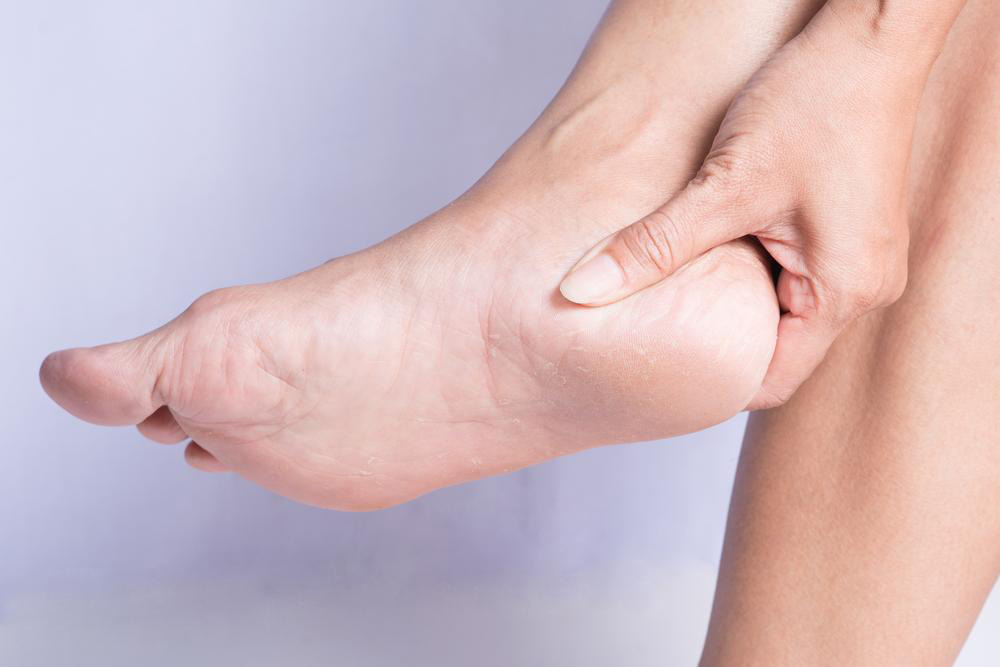
Effective Heel Spur Management: Causes, Symptoms, and Comprehensive Treatment Options
Heel spurs are bony growths on the heel caused by calcium deposits resulting from repetitive stress and injury. This comprehensive guide explores their causes, symptoms, and effective treatment options, including conservative therapies and surgical procedures. Preventive tips emphasize proper footwear, regular foot care, and lifestyle modifications. Whether you are experiencing mild discomfort or chronic pain, understanding heel spurs can help you manage the condition effectively. Enhancing foot health through targeted exercises, diet, and professional care can significantly improve quality of life and prevent recurrence of heel spur issues.
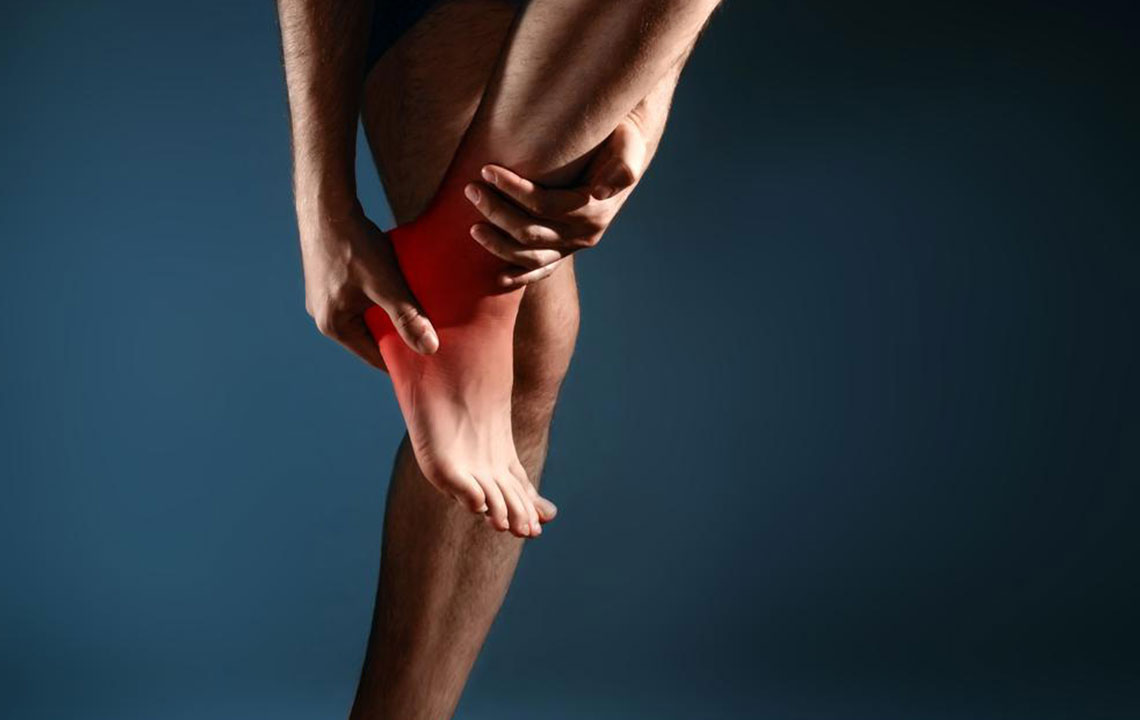
Effective Heel Spur Management: Causes, Symptoms, and Comprehensive Treatment Options
Heel spurs are bony growths that develop on the underside of the heel bone, often causing discomfort and pain. These calcified deposits form due to prolonged calcium buildup in response to repetitive stress or injury to the plantar fascia—the thick band of tissue connecting the heel bone to the toes. Heel spurs are a common condition among athletes, runners, and individuals with active lifestyles, but they can also affect anyone experiencing prolonged strain or abnormal biomechanics of the foot. Understanding the causes, recognizing the symptoms, and exploring available treatment strategies are crucial for effective management and relief.
Understanding the underlying causes of heel spurs—
Heel spurs develop gradually over months or even years as a result of repetitive stress and micro-injuries to the foot's soft tissues. When the plantar fascia experiences excessive tension or is repeatedly strained—such as during high-impact activities or prolonged standing—the body's natural response is to deposit calcium where the tissues are damaged or torn. This calcium accumulation over time forms the spur. Additional factors that increase the likelihood of heel spur formation include being overweight, which places additional stress on the heel and foot arch, gait abnormalities like overpronation or supination, and wearing improperly fitted footwear lacking adequate arch support or cushioning. Occasionally, improper walking mechanics or flat feet can contribute to uneven stress distribution across the heel, accelerating spur development. Chronic conditions like plantar fasciitis, which involves inflammation of the plantar fascia, are often associated with heel spur formation, making it a common coexisting condition.
Recognizing the symptoms associated with heel spurs—
Many individuals with heel spurs may not initially experience noticeable symptoms, as the spur itself can be asymptomatic. However, when symptoms do occur, they often manifest as a sharp, stabbing pain localized to the bottom or back of the heel. This pain tends to worsen with weight-bearing activities such as walking, running, or standing for extended periods. Morning pain or stiffness when first getting out of bed is a classic symptom, often easing after a few minutes of movement. Nonetheless, pain may recur after prolonged activity or rest. The discomfort is frequently related to associated soft tissue injuries, like plantar fasciitis or inflammation around the spur, rather than the spur itself directly irritating the tissues. Some patients also report a feeling of tenderness or swelling around the heel, especially after activity.
Types of heel spurs—
Heel spurs can be classified based on their location on the heel. The most common are posterior inferior spurs, which occur beneath the heel and are typically linked to plantar fasciitis. Another type includes posterior superior spurs, positioned near the back of the heel and close to where the Achilles tendon attaches. The specific type of spur may influence the severity of symptoms and guide treatment choices. Although imaging techniques like X-rays confirm the presence of a heel spur, treatment focuses on alleviating symptoms since the spurs themselves are often not the direct cause of pain but a sign of underlying issues.
Available treatments for heel spurs—
Conservative Management Strategies: For mild to moderate cases, non-surgical approaches typically provide significant relief. Physical therapy aimed at stretching and strengthening the Achilles tendon and plantar fascia can reduce tension and prevent further injury. Custom orthotics or heel inserts help distribute pressure evenly across the foot and cushion the heel. Heel cups and straps can provide additional support and reduce stress on inflamed tissues. Supportive footwear that absorbs shock and offers stability is recommended; for example, shoes with firm arch support and cushioning soles are helpful. Over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs)—like ibuprofen or acetaminophen—can reduce pain and inflammation. Corticosteroid injections may be indicated for persistent inflammation, providing targeted relief. Most individuals respond well to these interventions, experiencing improved comfort and function.
Surgical Options: When symptoms persist despite rigorous conservative management over a period of 10-12 months, surgical intervention may be necessary. Surgical procedures typically involve removing the heel spur and releasing the plantar fascia if deemed appropriate. Some surgeons perform a plantar fasciotomy, which involves cutting part of the fascia to relieve tension. Post-operative care includes limited weight-bearing initially, the use of crutches or special footwear, and physical therapy to restore strength and flexibility. While surgery can significantly reduce pain, it carries potential risks, including nerve injury, infection, scarring, or recurrence of symptoms. Therefore, it’s essential to weigh benefits with possible complications and consider surgery only after comprehensive consultation with a healthcare professional.
Preventative measures to avoid heel spurs—
Prevention primarily involves maintaining good foot health and biomechanics. Selecting footwear that offers shock absorption, arch support, and a stable heel counter is key to minimizing abnormal stress on the heel. Runners should choose shoes with proper cushioning and transitioning gradually into high-impact activities to prevent overloading the foot structures. Warming up and stretching the Achilles tendon and plantar fascia before engaging in physical activities helps reduce strain. Maintaining a healthy weight alleviates excess pressure on the heel, decreasing the likelihood of spur formation. Replacing worn-out shoes regularly and practicing good foot hygiene are simple yet effective strategies to prevent heel problems. Incorporating foot exercises and strengthening routines can improve foot mechanics and reduce the risk of developing heel spurs.
Diet, lifestyle, and home remedies—
Adopting a diet rich in nutrients supporting bone and tissue health—such as magnesium, zinc, and silicon—can help maintain strong, healthy tendons and bones. Consuming bromelain-rich foods like pineapple and papaya may assist in reducing inflammation and swelling around the heel. Proper hydration and a balanced diet contribute to overall tissue repair and resilience. Regular foot massages, ice therapy, and stretching exercises can further alleviate symptoms and improve flexibility. Wearing supportive shoes, avoiding prolonged standing, and taking breaks during extended periods of activity are practical lifestyle modifications. These measures, coupled with aerobic activities that promote circulation, help mitigate heel stress and prevent spur development. If heel pain persists, consulting with a healthcare professional ensures accurate diagnosis and personalized treatment plan.