Comprehensive Guide to Managing and Treating Neuropathic Pain
This comprehensive guide explores effective strategies for managing neuropathic pain, including causes, symptoms, medication options, and lifestyle tips. It emphasizes early diagnosis, targeted treatments like medications and topical therapies, and preventive measures to maintain nerve health. Suitable for patients and caregivers, this article provides valuable insights into alleviating neuropathic discomfort and improving quality of life.
Effective Strategies for Managing Neuropathic Pain and Discomfort
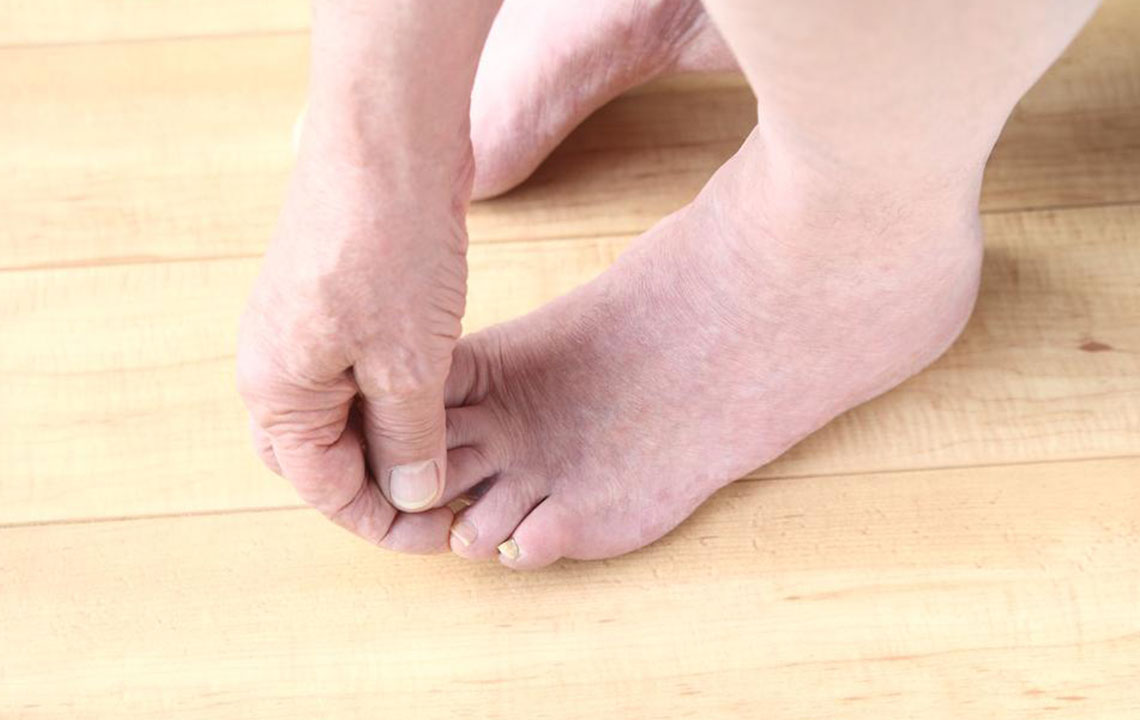
Neuropathic pain is a complex, often chronic condition that arises when nerve pathways are damaged or dysfunctional due to injury or medical disorders. This disruption in nerve signaling can lead to a variety of sensory disturbances, ranging from numbness and tingling to persistent burning or stabbing pain. Such symptoms not only diminish quality of life but also pose significant challenges in management. Understanding the underlying causes, symptoms, and available treatment options is essential for effective management and relief.
Neuropathic pain can develop from various underlying health conditions, including nerve compression syndromes like carpal tunnel syndrome, trauma, or degenerative diseases such as multiple sclerosis, HIV-related nerve damage, or diabetic neuropathy. Such conditions compromise nerve function, leading to abnormal pain signaling. Additionally, injuries to the brain or spinal cord can result in severe neuropathic symptoms, which are often challenging to treat. Recognizing the root cause of nerve damage is crucial for targeted therapy, making diagnosis an essential early step in treatment planning.
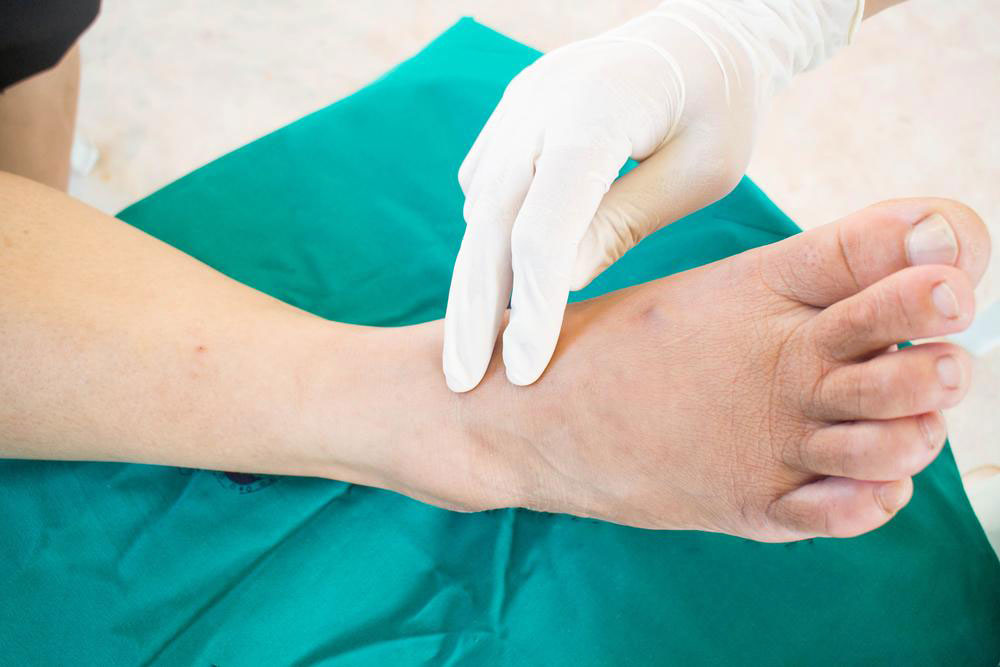
The symptoms of neuropathic pain can vary widely. Patients may experience a burning sensation, a stabbing or shooting pain, heightened sensitivity to touch (allodynia), or pain triggered by simple pressure or temperature changes. These sensations can be persistent or intermittent, often fluctuating in severity during the course of a day. Healthcare providers typically utilize pain assessment tools—such as numeric rating scales, visual analog scales, or facial expression charts—to evaluate pain intensity accurately. This assessment guides the development of personalized treatment strategies aimed at alleviating discomfort and improving function.
Medications for Neuropathic Pain Relief
Many pharmaceutical options are available for managing neuropathic pain, with some drugs being more effective depending on individual patient profiles. Antidepressants, particularly tricyclic antidepressants like amitriptyline, nortriptyline, and desipramine, have a long-standing history of reducing neuropathic symptoms. These medications help modulate neurological pathways involved in pain transmission. Selective serotonin reuptake inhibitors (SSRIs) such as citalopram and paroxetine are also used, especially when comorbid depression is present. Other antidepressants like bupropion and venlafaxine have shown promise in pain management.
Antiseizure drugs are commonly prescribed for nerve-related pain because they stabilize overactive nerve activity. Gabapentin and pregabalin are popular choices, reducing nerve excitability and providing relief. Carbamazepine, lamotrigine, and phenytoin are additional options, often used when other treatments are insufficient. The goal of medication therapy is to alleviate pain without significant side effects, necessitating careful selection and monitoring by healthcare providers. In some cases, combination therapy may be prescribed to improve efficacy.
Alternative and Adjunct Treatment Options
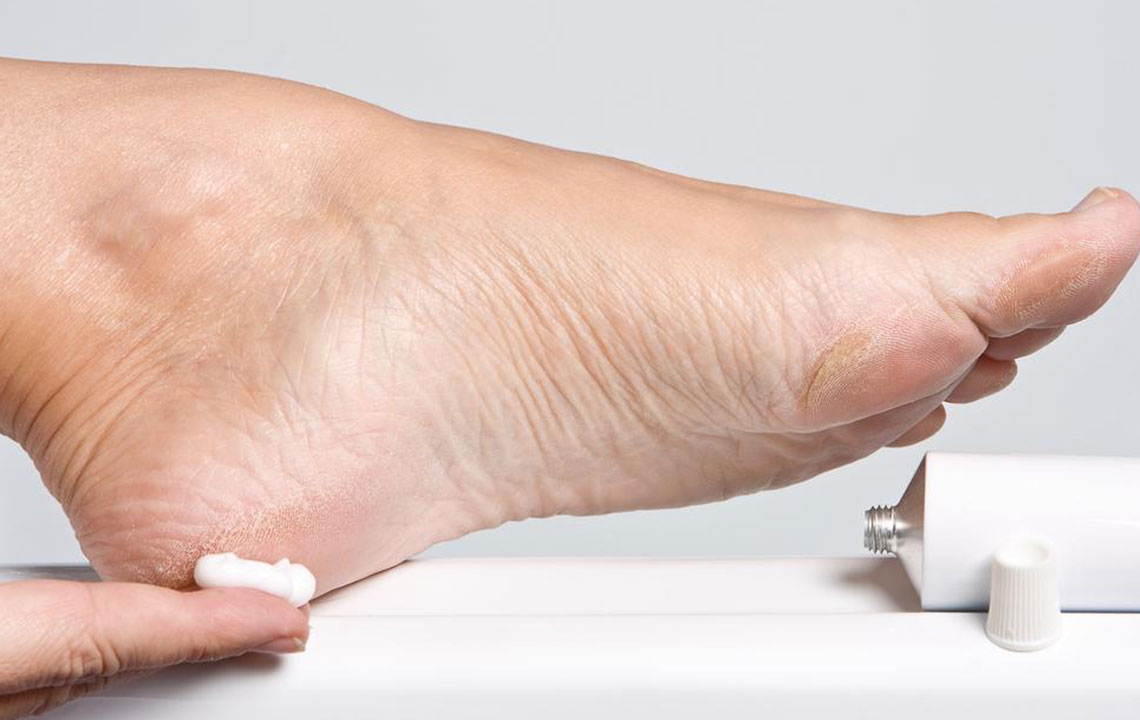
Topical therapies offer a safe, targeted approach for symptom relief. Capsaicin patches and gels, which contain an active component derived from chili peppers, work by desensitizing sensory nerves over time, leading to reduced pain signals. Lidocaine patches are another option, providing localized numbing effects to diminish discomfort. While narcotic medications (opioids) are sometimes considered, they are generally avoided as first-line treatments due to risks of dependency, tolerance, and adverse effects. Addressing the underlying cause of neuropathy, when reversible, can promote nerve repair and reduce chronic pain.
Prevention Strategies and Lifestyle Modifications
Prevention and management of neuropathic pain heavily depend on lifestyle choices and early intervention. Maintaining a healthy lifestyle by limiting alcohol intake, avoiding smoking, and managing body weight can significantly reduce the risk of nerve damage. Practicing ergonomic techniques, especially for repetitive tasks, minimizes strain on nerves, preserving their integrity. Regular health screenings are vital, particularly for conditions like diabetes, which is a leading cause of neuropathy. Tight blood sugar control and early treatment of nerve injuries can mitigate the severity of symptoms. If neuropathy develops, timely medication and supportive therapies can help control symptoms and improve quality of life.