Comprehensive Guide to Managing Crohn’s Disease: Symptoms, Causes, and Treatment Options
Explore an in-depth guide to Crohn’s disease, covering its symptoms, causes, and modern treatment options. Learn how early diagnosis and personalized management strategies can improve quality of life for those affected by this chronic inflammatory bowel condition. This comprehensive overview highlights current therapies and future prospects in Crohn’s disease care.
Understanding Crohn’s Disease: Key Facts and Insights
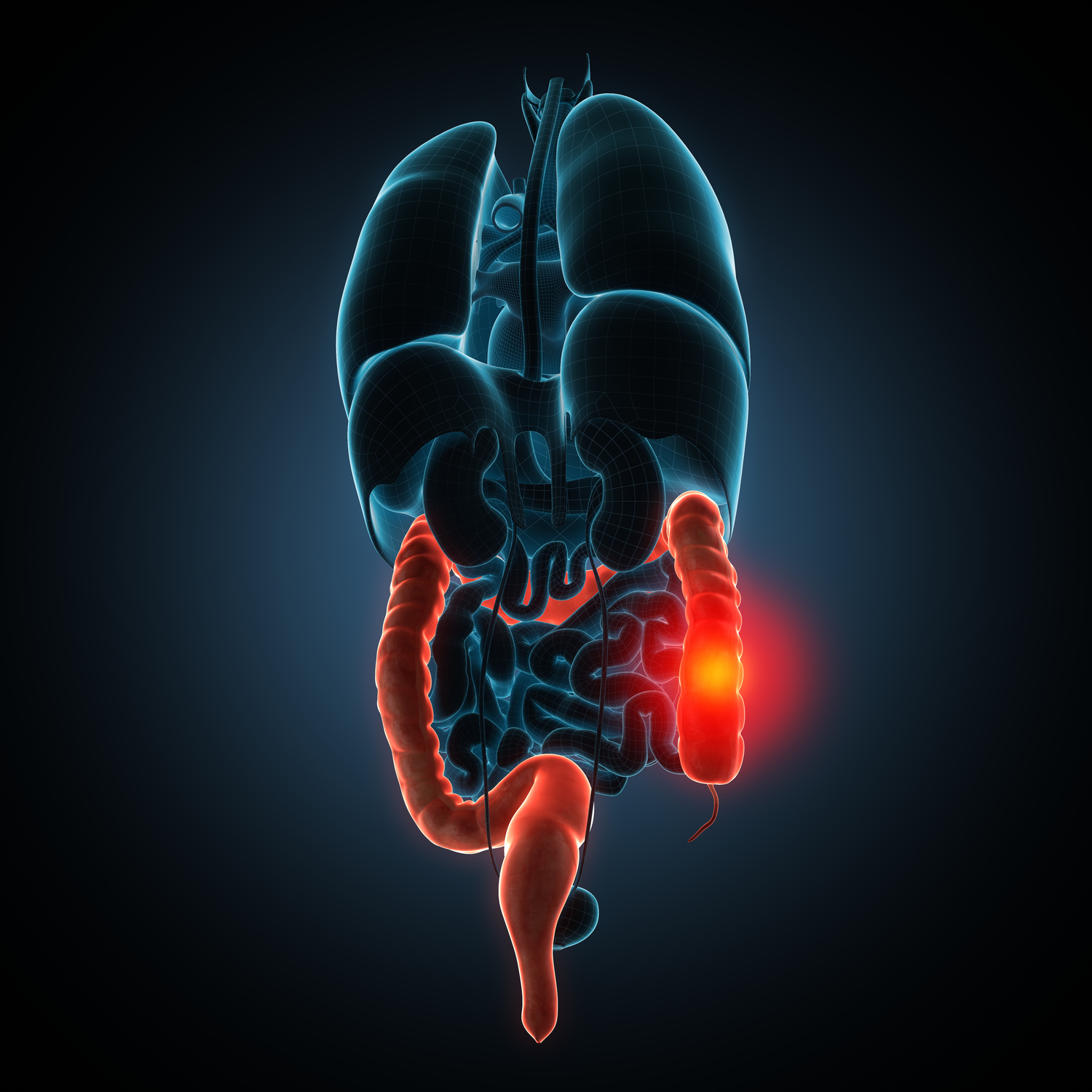
Crohn’s disease is a chronic inflammatory condition that primarily affects the gastrointestinal (GI) tract, classified under the category of inflammatory bowel diseases (IBD). It can cause severe inflammation, leading to a wide array of symptoms that significantly impact a person's daily life and overall health. This article provides an in-depth exploration of Crohn’s disease, including its causes, symptoms, complications, and current management strategies aimed at improving quality of life for those affected.
As one of the most challenging disorders within the realm of digestive health, understanding Crohn’s disease is crucial for early diagnosis, effective treatment, and ongoing management. The condition can affect any part of the GI tract from the mouth to the anus, but it most commonly impacts the terminal ileum—the last part of the small intestine—and the colon. Its unpredictable nature, variable severity, and potential for complications make it a significant concern for patients worldwide.
Key Symptoms and Signs of Crohn’s Disease
Recognizing the symptoms of Crohn’s disease early is vital for prompt diagnosis and treatment. Depending on the affected regions and disease severity, symptoms can persist for extended periods, ranging from weeks to years. Common clinical signs include:
Persistent Diarrhea: Diarrhea is often the most prominent symptom. When the small intestine is inflamed, it produces watery stools, whereas colon involvement can lead to bloody diarrhea. During flare-ups, symptoms may become more intense and frequent.
Rectal Bleeding: Spotting blood in stool, which often appears bright red, indicates bleeding within the rectum or large intestine. Severe bleeding episodes can be life-threatening and require urgent medical attention.
Fever and Night Sweats: These systemic symptoms develop as the immune system responds to ongoing inflammation, affecting overall body temperature and causing sweating during nighttime.
Chronic Fatigue: Due to persistent blood loss and nutritional deficiencies, patients often experience profound fatigue, weakness, and reduced stamina. Sleep disturbances related to discomfort further exacerbate tiredness.
Abdominal Pain and Cramping: Inflammation within the GI tract leads to cramps, tenderness, and discomfort, especially during active disease phases, often associated with diarrhea episodes.
Loss of Appetite and Nausea: Discomfort, pain, and nausea can diminish the desire to eat, resulting in reduced caloric intake and potential malnutrition.
Unintentional Weight Loss: The combination of decreased appetite, malabsorption of nutrients, and increased metabolic demands due to inflammation leads to significant weight loss, muscle wasting, and protein deficiency.
Fistula Formation and Abscesses: Chronic inflammation can cause abnormal connections (fistulas) to develop between different parts of the bowel or between the bowel and other organs, potentially leading to infections and abscesses, especially around the anal region.
Gastrointestinal Ulcers: Ulcers may form throughout the digestive tract, causing further pain, bleeding, and complications.
As Crohn’s disease progresses, additional health issues may arise, including inflammation in joints (arthritis), skin rashes, eye problems, liver disease, and delayed growth or puberty in pediatric patients. Persistent and worsening symptoms demand ongoing medical evaluation, as untreated disease can lead to severe complications.
Understanding the Causes and Risk Factors
The precise cause of Crohn’s disease remains elusive, but current research suggests a multifactorial origin involving genetic, environmental, and immune system components. It is believed that an abnormal immune response triggers inflammation in the gastrointestinal tract, attacking healthy tissue instead of pathogens. This dysregulated immune activity may be influenced by genetic predisposition—familial history of IBD increases the risk.
Environmental factors such as smoking, diet, and sanitation levels also play roles in disease development. Certain bacteria or infections may act as triggers in susceptible individuals, setting off the immune response that results in chronic inflammation. Despite extensive research, the exact etiology continues to be a subject of scientific investigation.
Current Management and Treatment Strategies
Although there is no known cure for Crohn’s disease, significant advancements in treatment have improved patient outcomes and quality of life. The primary goals are to reduce inflammation, manage symptoms, prevent complications, and promote remission. Treatment plans are highly individualized, often combining medication, nutritional support, and sometimes surgical intervention.
Medications commonly prescribed include:
Anti-inflammatory drugs: Such as aminosalicylates, which help control mild inflammation.
Corticosteroids: Utilized to achieve quick symptom relief during flare-ups but are not suitable for long-term use due to side effects.
Immunomodulators: Medications like azathioprine and methotrexate suppress immune activity to reduce inflammation.
Biologic therapies: Target specific immune molecules (e.g., TNF-alpha inhibitors) to control severe or refractory cases.
Antibiotics: Sometimes used to treat or prevent infections, abscesses, and fistulas.
In addition to medication, nutritional therapy can help manage symptoms and correct deficiencies. Special diets or elemental formulas may be recommended to reduce bowel activity and support healing. Maintaining hydration and electrolyte balance is also crucial.
Surgical options are considered when medical therapy fails or complications like strictures, fistulas, or perforation occur. Procedures range from removing damaged sections of the bowel to creating stomas or other diversion surgeries.
Living with Crohn’s disease requires ongoing management, including regular checkups, lifestyle modifications, stress management, and avoiding triggers like smoking or certain foods. Emerging therapies and ongoing research continue to improve the outlook for patients and aim for potential cures in the future.
In conclusion, understanding Crohn’s disease’s complexities enables patients and healthcare providers to work collaboratively towards effective control and improved life quality. Early detection, personalized treatment, and lifestyle adjustments remain the cornerstones of managing this challenging condition effectively.