Comprehensive Guide to Lupus Skin Rash: Recognizing Symptoms and Effective Management Tactics
This comprehensive guide explores lupus skin rash, detailing its symptoms, including rash, joint pain, hair loss, and systemic involvement. It emphasizes the importance of early diagnosis through blood tests and highlights effective treatment options such as medication, lifestyle changes, and sun protection. The article provides practical tips for managing flare-ups, highlights potential organ complications, and offers strategies to improve quality of life for individuals living with lupus. Understanding these aspects is vital for early intervention and optimal disease management, helping patients lead healthier, more active lives.
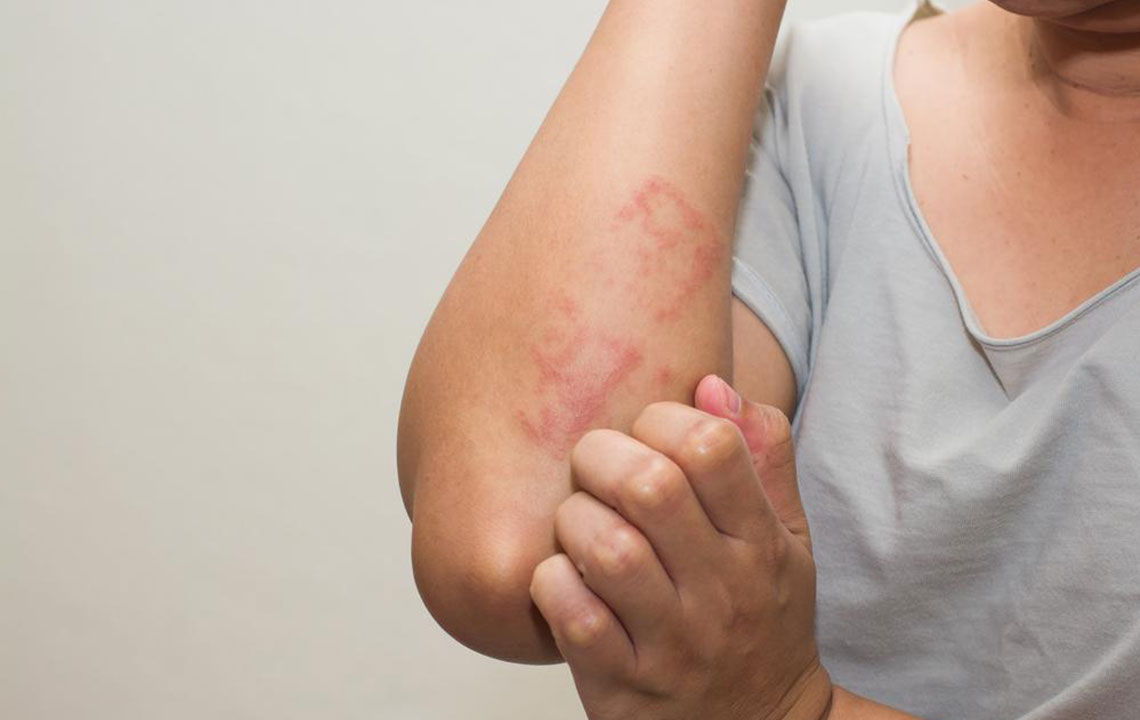
Comprehensive Guide to Lupus Skin Rash: Recognizing Symptoms and Effective Management Tactics
Lupus skin rash is a complex autoimmune disorder that manifests through a variety of skin-related symptoms, often accompanied by other systemic signs. This condition arises when the immune system mistakenly attacks healthy skin tissues, leading to inflammation, discomfort, and visible skin changes. Although lupus can develop at any age, it most commonly begins to appear in early adulthood, typically around the age of thirty. It predominantly affects women, with men being less frequently diagnosed. The disease course varies from mild to severe, with fluctuations between flare-ups and remission phases. Currently, there is no definitive cure for lupus; however, a combination of medical treatments and lifestyle modifications can significantly alleviate symptoms, reduce disease activity, and enhance overall quality of life.
Key Indicators and Symptoms of Lupus Skin Rash
Understanding the primary signs of lupus skin involvement is crucial for early detection and management. Typical indicators include persistent rash, unexplained fever, hair thinning or loss, fatigue, inflammation of internal organs such as kidneys, joint pain, dryness in the mouth, thyroid irregularities, and digestive disturbances. Recognizing these symptoms can prompt timely medical intervention to control disease progression.
Nail Changes and Skin Manifestations
Individuals with lupus may notice changes in their nails, such as discoloration, brittleness, cracking, or even falling off. Red spots within the nail beds may also appear due to inflammation of blood vessels. The hallmark skin presentation is the butterfly-shaped rash (malar rash), spanning across the cheeks and bridge of the nose, often accompanied by red spots, mouth ulcers, and purplish rashes. These skin changes tend to worsen with sun exposure or certain triggers.
Hair Loss and Sensitivity to Light
Hair thinning, scalp flakes, and patchy hair loss are common among lupus patients. Photosensitivity is another prominent feature, where exposure to sunlight or artificial ultraviolet light exacerbates skin rashes and can cause new lesions to develop. Patients are advised to minimize sun exposure and adopt sun-protection strategies to prevent flare-ups.
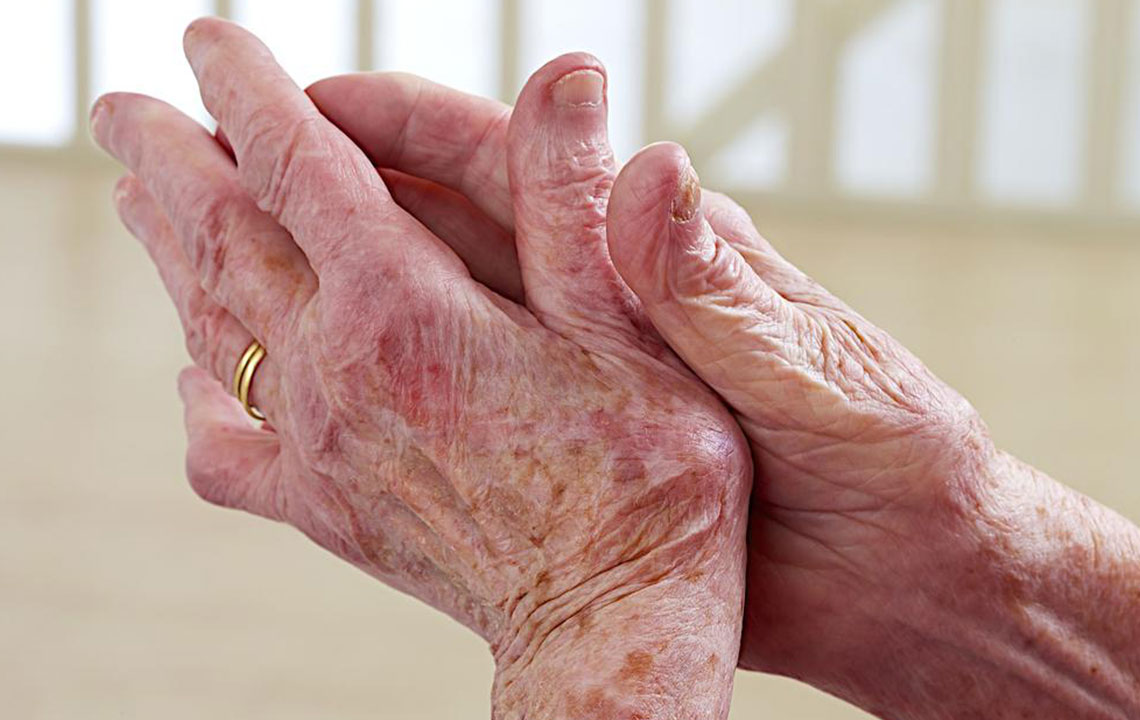
Joint and Systemic Symptoms
Early manifestations often include joint discomfort, swelling, and stiffness affecting wrists, fingers, knees, and other joints. Mild muscle inflammation may also occur, contributing to general discomfort. Additionally, many patients experience fevers ranging from low-grade to high, along with feelings of fatigue and exhaustion that impair daily activities, including walking and other movements.
Raynaud’s Phenomenon and Circulatory Issues
Raynaud’s phenomenon, characterized by numbness and color changes in fingers and toes, is another common symptom. Blood vessel constriction in response to cold or stress causes the affected areas to turn white or blue, and then red upon rewarming. This condition highlights the vascular involvement in lupus and can lead to further complications if left unmanaged.
Diagnosis and Laboratory Assessments
Diagnosing lupus involves comprehensive blood panels to detect antinuclear antibodies (ANA), as well as tests to evaluate organ function, inflammation markers, and tissue biopsies in certain cases. Early diagnosis is essential for controlling disease activity and preventing long-term organ damage. Regular monitoring helps adapt treatment plans to the patient's evolving condition.
Management and Treatment Strategies
The primary approach to managing lupus skin rash includes medications such as anti-inflammatory drugs, corticosteroids to reduce inflammation, and antimalarial agents like hydroxychloroquine to modulate immune responses. Adjunct therapies include immunosuppressants in severe cases. Alongside pharmacologic treatments, lifestyle modifications play a vital role in controlling flare-ups and maintaining well-being.
Lifestyle Modifications and Self-Care
Adapting daily routines helps manage symptoms effectively. Regular exercise improves circulation and reduces fatigue, while sufficient sleep and stress management—through yoga, meditation, and relaxation techniques—help stabilize immune function. Protecting skin from sun exposure with high-SPF sunscreens, protective clothing, and seeking shade are critical preventive measures.
Impact on Organs and Long-Term Health Risks
Prolonged lupus can affect vital organs, leading to complications such as kidney inflammation (lupus nephritis), which may cause swelling, high blood pressure, and impaired kidney function. Cardiac involvement, including inflammation of the pericardium (pericarditis) and arteries, can result in chest pain and cardiovascular risks. Lung inflammation may cause difficulty breathing, and digestive issues like nausea, abdominal pain, and weight loss can occur as systemic effects of the disease. Proper medical management is essential to minimize these risks and preserve organ health.
Credits: Effective management of lupus requires a multidisciplinary approach involving dermatologists, rheumatologists, and primary care providers. Patients benefit from education about disease triggers, medication adherence, and monitoring to maintain a balanced, healthier life.