Complete Overview of Atrial Fibrillation: Causes, Treatments, and Preventive Strategies
This extensive guide provides insights into atrial fibrillation, its symptoms, and the latest management strategies. It covers medications, surgical options, and lifestyle changes crucial for preventing complications like strokes and improving quality of life. Tailored treatment plans and early intervention are emphasized to achieve optimal health outcomes for AFib patients. Whether you are newly diagnosed or seeking to better understand AFib, this article is a valuable resource for comprehensive care and effective management.

Understanding Atrial Fibrillation and Exploring Its Treatment Options
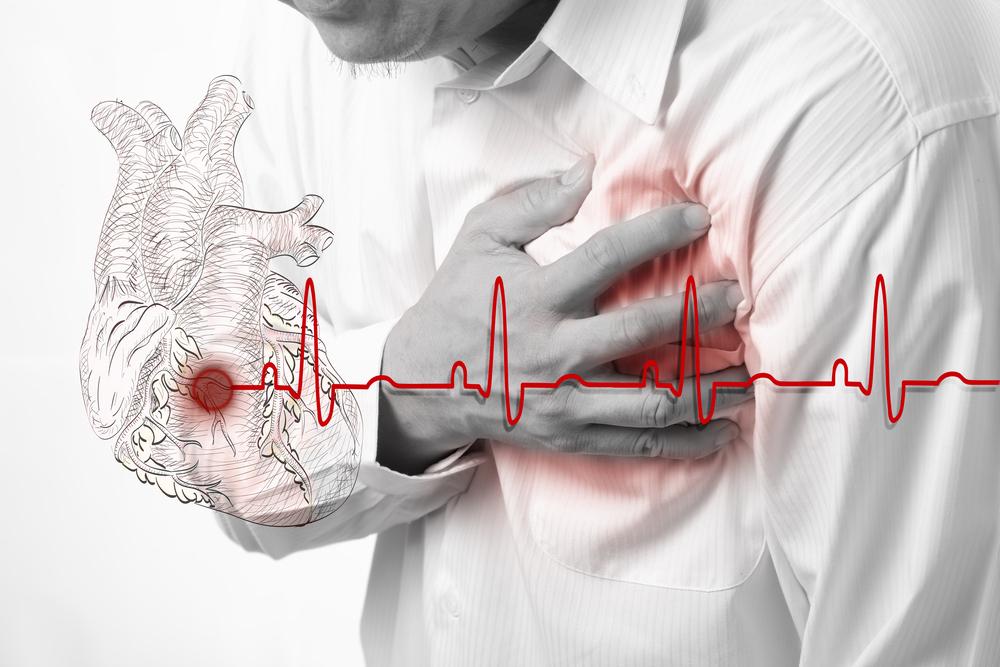
Atrial fibrillation (AFib), also known as AF, is one of the most common cardiac arrhythmias encountered in clinical practice. This condition manifests as an irregular and often rapid heartbeat originating from disorganized electrical activity in the heart's atria—the upper chambers of the heart. The impact of AFib extends beyond mere irregular rhythms; it significantly increases the risk of life-threatening events such as stroke, blood clot formation, and even heart failure if left untreated. Globally, it is estimated that over 2.7 million people are affected by AFib, many of whom remain unaware of their condition due to only subtle or absent symptoms. Early detection and comprehensive management are crucial to reducing the potential for severe complications and enhancing patient quality of life.
The hallmark signs and symptoms of atrial fibrillation can vary widely among individuals. Common manifestations include palpitations—an abnormal awareness of heartbeats—shortness of breath, fatigue, chest discomfort, dizziness, and weakness. Interestingly, some patients may be entirely asymptomatic, with the condition only being discovered during routine medical examinations or evaluations for unrelated health issues. This underscores the importance of regular checkups and screening, especially in individuals with risk factors such as advanced age, hypertension, or a history of cardiovascular disease.
Strategies for Managing Atrial Fibrillation
Time elapsed since diagnosis
Underlying causes and contributing factors
Severity and frequency of symptoms
The overarching objectives in AFib treatment are to prevent the formation of blood clots that can lead to strokes, regulate the heart rate to restore normal rhythm, and minimize the risk of embolism and other complications. To achieve these goals, a combination of medications, surgical procedures, and lifestyle modifications are employed tailored to each patient’s specific needs and clinical presentation.
Medications for Atrial Fibrillation
Pharmacological treatment plays a central role in AFib management. Blood thinners, also known as anticoagulants, are prescribed to reduce the tendency of blood clot formation. Common anticoagulant drugs include warfarin and the newer direct oral anticoagulants such as rivaroxaban, dabigatran, apixaban, and edoxaban. These agents help lower the risk of stroke significantly. Additionally, rate-control medications like atenolol, metoprolol, and propranolol are used to slow down the heart rate, making it more manageable. Rhythm stabilizers—including flecainide, amiodarone, and sotalol—are employed to maintain or restore normal heart rhythm in selected patients.
Surgical and Minimally Invasive Procedures
For certain cases, especially when medications are insufficient or not well-tolerated, surgical interventions become necessary. Pacemaker implantation can help regulate abnormal heartbeats, while maze surgery creates scar tissue in the atria to block aberrant electrical pathways. Catheter ablation, a minimally invasive technique, involves threading catheters through blood vessels to targeted areas within the heart to destroy faulty electrical pathways responsible for AFib. This approach has shown high efficacy in selected patients and can significantly reduce symptoms and episodes.
Non-Invasive Treatment Methods
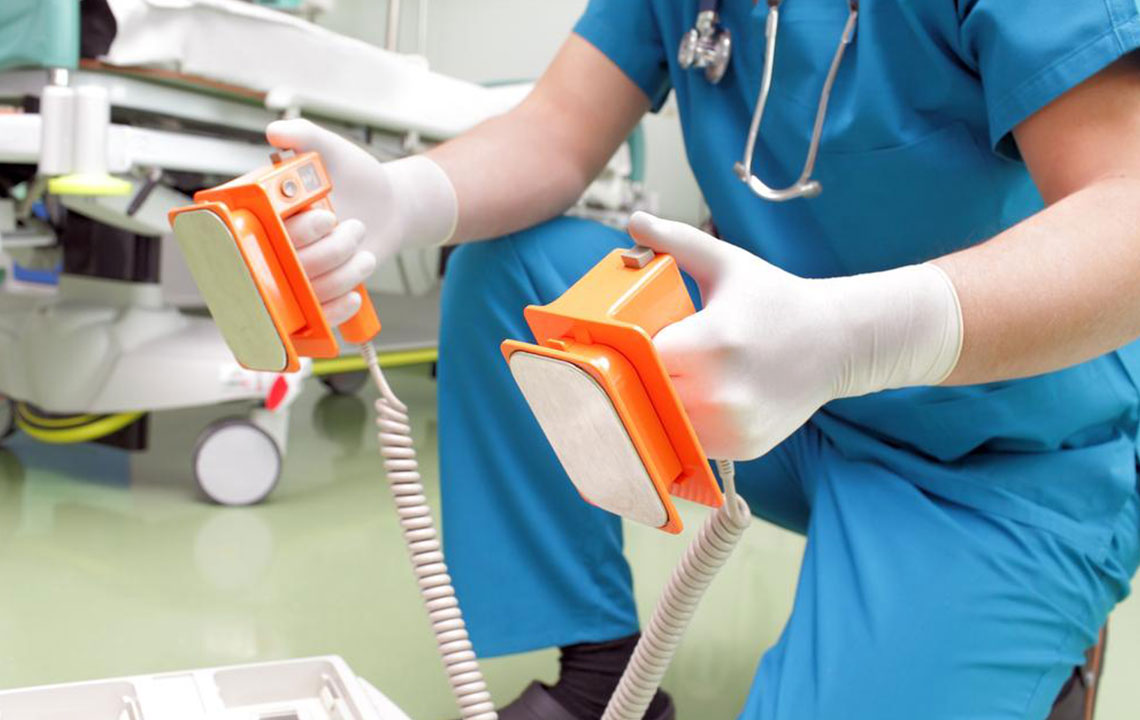
Procedures like electrical cardioversion and radiofrequency ablation are frequently performed in hospital settings. Electrical cardioversion involves delivering a controlled electric shock to the heart to restore normal rhythm, often performed under sedation. Radiofrequency ablation employs heat generated by radio waves to selectively destroy areas causing irregular electrical signals. Both procedures are generally safe and can provide long-term relief from symptoms when appropriately indicated.
Lifestyle Changes and Preventive Measures
Adopting a heart-healthy lifestyle is vital in managing AFib and preventing its progression. Regular physical activity, a balanced diet low in saturated fats and sodium, quitting smoking, and maintaining an ideal body weight can considerably improve cardiac health. Managing stress through relaxation techniques and avoiding stimulants like caffeine can also play a role in symptom control. Patients with AFib are encouraged to monitor their symptoms closely and adhere to prescribed medication regimens. Early medical consultation upon noticing any new or worsening symptoms is essential to prevent adverse events and optimize treatment outcomes.
During comprehensive management, collaboration between cardiologists, primary care physicians, and allied health professionals ensures that each patient receives personalized care aimed at minimizing risks and improving overall well-being.