Comprehensive Guide to Bariatric Surgery: Benefits, Risks, and Essential Facts
This comprehensive guide explores bariatric surgery, detailing its types, benefits, potential risks, and essential considerations for patients. Discover how these procedures can significantly improve health outcomes, reduce obesity-related conditions, and what to expect before and after surgery to ensure success.
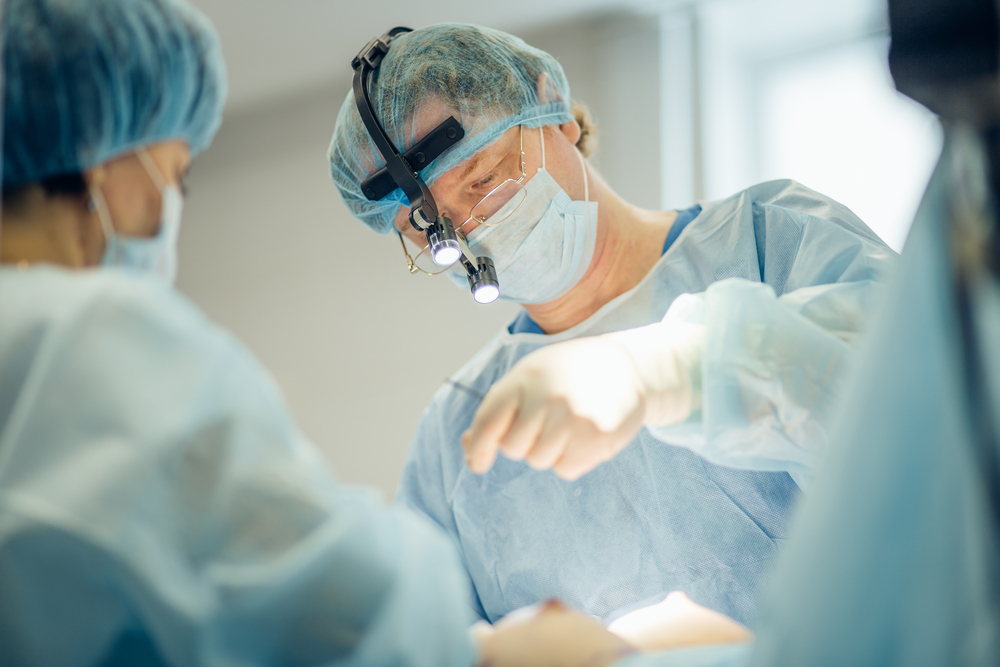
Comprehensive Guide to Bariatric Surgery: Benefits, Risks, and Essential Facts
Bariatric surgery, widely recognized as a powerful medical intervention for weight loss, has transformed the lives of countless individuals struggling with obesity. As the obesity epidemic continues to rise globally, more patients are exploring surgical options to improve their health outcomes and quality of life. This article provides an in-depth overview of bariatric procedures, including their types, benefits, potential risks, and the critical considerations prospective patients should keep in mind before undergoing surgery.
The fundamental goal of bariatric surgery is to induce significant and sustained weight loss, which often results in the improvement or remission of serious health conditions such as type 2 diabetes, hypertension, sleep apnea, and hyperlipidemia. These health benefits have made bariatric surgery a preferred solution for those failing to achieve sufficient weight loss through traditional methods like dieting and exercise.
Cost is a significant consideration for many individuals contemplating bariatric surgery. Fortunately, many health insurance plans now recognize the medical necessity of these procedures and provide substantial coverage, reducing the financial burden on patients. Nonetheless, it remains essential for prospective candidates to verify their insurance policies and understand the coverage details beforehand.
Ideal candidates for bariatric surgery typically include individuals who have struggled with severe obesity despite attempting various non-surgical weight loss methods. Patients with a body mass index (BMI) of 40 or higher, or those with a BMI of 35 or higher accompanied by obesity-related health issues, are often considered for surgery. Additionally, candidates should be committed to lifestyle changes, including dietary modifications and regular physical activity, to ensure long-term success.
Bariatric surgeries encompass a range of procedures, each with specific mechanisms, benefits, and risks. The most common types include:
Gastric Bypass (Roux-en-Y)
This involves creating a small stomach pouch and bypassing a segment of the small intestine, leading to reduced food intake and nutrient absorption. It’s considered highly effective but involves a more complex surgical process.
Sleeve Gastrectomy
The surgeon removes a large portion of the stomach, leaving a tubular or sleeve-shaped stomach. This procedure limits food intake and decreases hunger hormones, offering significant weight loss outcomes with less complexity.
Biliopancreatic Diversion with Duodenal Switch
A complex procedure combining sleeve gastrectomy with intestinal rerouting, providing substantial weight loss but with higher nutritional deficiency risks.
While bariatric surgery offers numerous benefits, it is essential to recognize and understand the potential side effects and complications associated with these procedures. Awareness and proper management can significantly mitigate risks and enhance recovery and long-term success.
Potential Side Effects and Complications
Dumping Syndrome
Also known as rapid gastric emptying, dumping syndrome occurs when food moves too quickly from the stomach into the small intestine. Symptoms can include nausea, dizziness, sweating, abdominal cramping, diarrhea, and fatigue. Patients are advised to modify their dietary intake to manage this condition effectively.
Hypoglycemia
Low blood sugar episodes can develop several years after surgery, particularly in patients with diabetes. Symptoms may involve shaking, confusion, sweating, weakness, and in severe cases, seizures. Regular monitoring and dietary adjustments are crucial for prevention.
Gallstones
Rapid weight loss increases the risk of gallstone formation. Patients may require additional treatment if gallstones cause pain or complications.
Internal Hernias
These occur when parts of the intestine protrude through internal openings or adhesions created during surgery, potentially leading to bowel obstruction. This complication is more common in open surgeries compared to minimally invasive laparoscopic procedures.
In addition to these risks, other potential complications include nutritional deficiencies, bleeding, infection, and adverse reactions to anesthesia. Therefore, thorough preoperative evaluation by a qualified bariatric surgeon and close postoperative monitoring are vital for ensuring safety and optimal outcomes.
Preparing for bariatric surgery involves comprehensive preoperative assessments, including nutritional counseling, psychological evaluation, and medical testing. Post-surgery, patients must adhere to prescribed dietary guidelines, attend follow-up appointments, and embrace lifestyle changes to sustain weight loss and health benefits.
In conclusion, bariatric surgery represents a significant medical advancement with the potential to radically improve health and quality of life for individuals battling severe obesity. With careful consideration of the benefits and risks, and under the guidance of experienced healthcare professionals, patients can achieve remarkable long-term health improvements through appropriately selected surgical interventions.





